Can Dental Whitening Strips Damage Teeth?
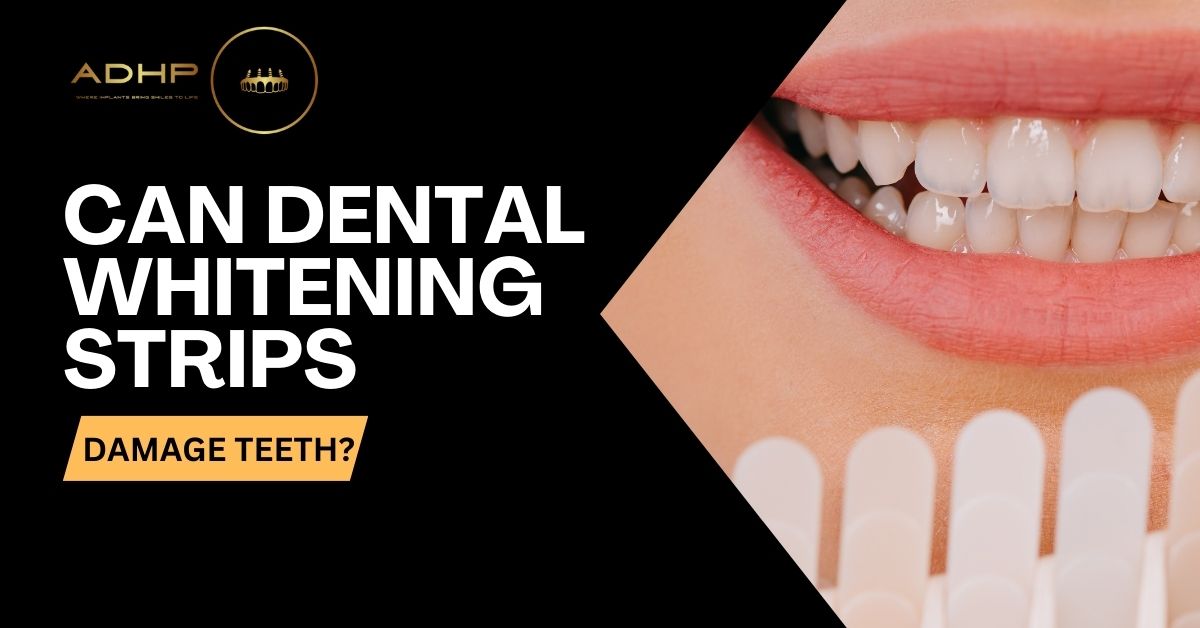
Main Takeaways: Whitening strips work by using peroxide to break down stains on tooth enamel, making teeth appear whiter. Overuse or incorrect use can lead to sensitivity, gum irritation, enamel erosion, and uneven whitening. Watch for warning signs like lingering sensitivity, gum pain, sharp toothaches, or enamel changes—stop use and see a dentist if they occur. Avoid use if you have sensitive teeth, gum disease, cavities, dental work, or are pregnant/nursing—always check with your dentist first. Safer whitening options include professional treatments, whitening toothpaste/mouthwash, and lifestyle changes to prevent stains. See your dentist first to check for dental issues and get personalized, safe whitening recommendations. Maintain your results with good oral hygiene, a stain-conscious diet, and occasional touch-ups as needed. Everyone wants a bright, sparkling smile. It makes you feel good and can boost your confidence. With so many products promising whiter teeth, whitening strips are a popular choice. They’re easy to use and seem to offer quick results right at home. But if you’re thinking about trying them, a big question might pop into your head: can whitening strips damage teeth? Let’s dig into that and figure out how to get a brighter smile safely. How Whitening Strips Work (The Basics) Before we talk about damage, it helps to know what whitening strips actually do. Most whitening strips have a thin layer of gel on them. This gel contains special ingredients, usually hydrogen peroxide or carbamide peroxide. These are the same kinds of ingredients dentists use for professional whitening, just in lower amounts. When you stick the strip to your teeth, the peroxide gel sits against your tooth enamel. Enamel is the hard, outer layer of your teeth. Over time, things like coffee, tea, red wine, and certain foods can stain this enamel, making your teeth look dull or yellow. The peroxide in the strips works like a tiny bleach. It gets into the enamel and breaks down the molecules that cause stains, making them less visible. This makes your teeth appear whiter. The strips are designed to be thin and flexible, so they fit snugly on your teeth. You usually wear them for a certain amount of time each day, as directed by the package, for a set number of days or weeks. It sounds simple, but understanding this process is key to figuring out, can whitening strips damage teeth? The Big Question: Can Whitening Strips Damage Teeth? So, back to our main question: can whitening strips damage teeth? The short answer is, it’s possible, especially if you don’t use them correctly. While most people use them without major issues, there are some risks to be aware of. The main concerns usually come from the peroxide in the strips. While it’s great at breaking down stains, it’s also a powerful chemical. Tooth Sensitivity: This is the most common side effect. You might feel a tingly or sharp pain in your teeth, especially when eating or drinking something hot or cold. This happens because the peroxide can temporarily make tiny tubes in your tooth enamel more open, exposing the sensitive inner part of your tooth. For most people, this sensitivity is temporary and goes away after they stop using the strips. But for some, it can be quite uncomfortable. Gum Irritation: Sometimes, the whitening gel can get onto your gums. Because gums are softer than teeth, the peroxide can irritate them, making them look white or inflamed. This is usually temporary, but it can be painful and might be a sign you’re not applying the strips correctly or that they’re too strong for your gums. Enamel Erosion (Rare but Serious): This is a more serious concern, though it’s less common with proper use. If you use whitening strips too often, for too long, or if the product is too strong, there’s a small risk that the peroxide could start to wear away your tooth enamel. Enamel does not grow back. Once it’s gone, it’s gone. Thinning enamel can lead to permanent sensitivity, make your teeth look more yellow (because the darker layer underneath shows through), and increase your risk of cavities. Uneven Whitening: Strips are flat, and teeth aren’t. They might not cover every curve or gap on your teeth perfectly. This can lead to a splotchy or uneven white appearance. Also, if you have dental work like fillings, crowns, or veneers, whitening strips won’t change their color. This means your natural teeth might get whiter, but your dental work will stay the same shade, leading to a noticeable mismatch. So, while whitening strips are generally considered safe for most people when used as directed, ignoring the instructions or overdoing it definitely increases the chance of problems. This is why knowing the answer to can whitening strips damage teeth is so important before you start. Signs of Trouble: When Whitening Strips Might Be Harming Your Teeth It’s helpful to know what signs to watch for if you’re worried about can whitening strips damage teeth. If you notice any of these, it’s a good idea to stop using the strips and talk to your dentist. Increased or Lingering Sensitivity: If your teeth become very sensitive to hot or cold, or if the sensitivity doesn’t go away after a day or two of not using the strips, that’s a warning sign. Gum Pain or Whitening: If your gums start to hurt, look irritated, or turn white where the strip has touched them, it means the peroxide is irritating your gum tissue. Sharp, Shooting Pains: While some dull sensitivity is common, sharp, sudden pains (especially when breathing in cold air or drinking) could signal more irritation to the tooth nerve. Changes in Enamel Texture: If your teeth feel rough, chalky, or look dull even after rinsing, it might be a sign of enamel changes. Dark Spots or Translucency: In very rare cases, if enamel is severely eroded, teeth might look more transparent at the edges, or underlying darker dentin might show through in spots. Existing Dental Issues Getting Worse: If you
Getting a Cavity Filled: Composite Filling

Main Takeaways Composite fillings are tooth-colored and made from a blend of plastic and glass, offering a natural look and strong bond to your tooth. They are a popular alternative to amalgam (silver) fillings because they preserve more of the natural tooth, bond directly, and contain no metal or mercury. The procedure involves removing decay, applying the composite in layers, and hardening it with a special light for a durable finish. With proper care, composite fillings typically last 5–10 years, depending on factors like location, oral hygiene, and chewing habits. Benefits include aesthetic appeal, conservative treatment, versatility, and less sensitivity to temperature changes compared to metal fillings. Drawbacks may include higher cost, longer placement time, potential staining, and slightly less durability in large, high-pressure fillings. Regular dental checkups, good oral hygiene, and avoiding hard foods help extend the life of your composite filling. ADHP – Torrance offers expert dental care and personalized guidance on choosing the right filling for your smile and needs. Nobody likes getting a cavity. That little hole in your tooth can be annoying, sometimes painful, and definitely something you want to fix. When you visit the dentist to get a cavity repaired, one of the most common solutions they offer is a composite filling. These tooth-colored fillings are popular for many reasons, but what exactly are they, and what should you know about them? Let’s talk about how these fillings work to fix your teeth and keep your smile looking great. What Exactly is a Composite Filling? When a dentist talks about a composite filling, they’re talking about a special kind of tooth repair that blends right in with your natural teeth. Unlike the old silver fillings (called amalgam fillings), composite fillings are made from a mix of plastic and fine glass particles. This mix can be colored to match the exact shade of your tooth, making it almost invisible when you smile. Think of it like this: when you have a cavity, it’s a hole caused by decay. The dentist first cleans out all the decayed (bad) part of your tooth. Then, they fill that space with the composite material. This material is soft at first, like a thick paste. The dentist shapes it to fit perfectly into the hole and match the natural curves of your tooth. Once it’s in place, they shine a special blue light on it. This light makes the composite material harden very quickly, becoming strong and durable. Because of its color-matching ability and the way it bonds to your tooth, a composite filling is a popular choice for fixing cavities, especially on your front teeth where they show, or even on back teeth where you want a natural look. Why Dentists Use Composite Fillings: The Big Benefits The reason so many dentists and patients choose a composite filling comes down to several important advantages. These fillings offer more than just fixing a hole; they help keep your smile looking its best. They Blend In: This is probably the biggest reason people love composite fillings. Since they can be matched to the exact color of your natural teeth, a composite filling is nearly invisible. You can laugh, talk, and smile wide without worrying about dark spots showing in your mouth. This is a huge plus, especially for cavities on front teeth or any part of your smile that people see. They Save More Tooth: With old silver fillings, dentists sometimes had to remove more healthy tooth material just to make sure the filling would stay in place. A composite filling actually bonds directly to the tooth structure. This means the dentist only needs to remove the decayed part of the tooth, leaving more of your healthy tooth untouched. Keeping more of your natural tooth is always better for the tooth’s long-term strength. They Bond to Your Tooth: The way composite material sticks directly to the tooth makes the tooth stronger. It helps support the remaining tooth structure and protects it from breaking. This bond also seals the tooth better, helping to keep out bacteria that could cause new decay under the filling. No Metal, No Mercury: Some people worry about the mercury content in old silver (amalgam) fillings. While dental organizations say amalgam fillings are safe, many people prefer a metal-free option. A composite filling offers this, as it contains no metal. This also means you don’t have to worry about the filling expanding and contracting as much with temperature changes, which could sometimes lead to cracks in your tooth with old metal fillings. Versatile Use: Besides filling cavities, composite material can also be used for other dental fixes. Dentists can use it to repair chipped or broken teeth, to fill in small gaps between teeth, or even to change the shape of teeth. This makes a composite filling a very flexible tool for improving smiles. These benefits make a composite filling a top choice for modern dental care, helping you keep both your oral health and your smile looking good. The Process: Getting a Composite Filling Getting a composite filling is a common and straightforward procedure that most people go through without much fuss. Here’s a step-by-step look at what happens during your dental visit: Numbing the Area: First, your dentist will usually numb the area around the tooth that needs work. They’ll use a local anesthetic, which is a special medicine that makes your tooth and gums feel sleepy, so you won’t feel any pain during the procedure. You might feel a small pinch when the shot goes in, but then the area will quickly go numb. Removing Decay: Once the area is numb, the dentist will carefully use a drill or other tools to remove all the decayed or damaged part of your tooth. They need to make sure every bit of the cavity is gone before they put in the new filling. Preparing the Tooth: After cleaning out the decay, the dentist will prepare the tooth surface. They might use a special gel or liquid
Bruxism Treatments: Finding Relief from Teeth Grinding and Jaw Pain

Main Takeways: Bruxism Basics: Bruxism is involuntary teeth grinding or clenching, often linked to stress, sleep disorders, or bite misalignment, and can cause tooth damage, jaw pain, and headaches. Common Symptoms: Look out for sore jaw muscles, worn or chipped teeth, tooth sensitivity, headaches, and sleep disturbances. Professional Treatments: Effective options include custom night guards, dental corrections, Botox injections, physical therapy, and treatment for underlying sleep issues. At-Home Solutions: Stress management, jaw exercises, warm compresses, avoiding stimulants, and improving sleep hygiene can help relieve symptoms. Children & Seniors: Bruxism affects all ages—kids may outgrow it, while seniors may need bite or denture adjustments due to age-related changes. Risks of Ignoring It: Untreated bruxism can lead to TMJ disorders, severe tooth wear, chronic pain, and reduced sleep quality. Why Choose ADHP – Torrance: Their expert team provides personalized, comprehensive bruxism treatment to relieve pain, restore function, and protect your long-term oral health. Do you wake up with sore jaw muscles, headaches, or worn-down teeth? You might be one of the millions of people affected by bruxism—a condition characterized by the involuntary grinding or clenching of teeth. While bruxism can affect people of all ages, it often goes undiagnosed until noticeable damage occurs. The good news? A wide range of effective bruxism treatments are available to help you find relief and protect your oral health. In this comprehensive guide, we’ll explore everything from the causes and symptoms of bruxism to the most effective professional and at-home treatment options. Whether your condition is mild or severe, there is a solution that can help you reclaim comfort, sleep better, and preserve your smile. What Is Bruxism? Bruxism is the medical term for the habitual grinding, gnashing, or clenching of teeth, typically occurring during sleep (sleep bruxism) or while awake (awake bruxism). Although occasional teeth grinding might not cause harm, chronic bruxism can lead to significant complications, including: Jaw pain and tension Tooth wear and fractures Headaches and migraines TMJ disorders Sleep disturbances Knowing what triggers bruxism is the first step toward identifying the best bruxism treatments for your specific needs. Causes of Bruxism: What’s Behind the Grinding? Bruxism can stem from a combination of physical, psychological, and genetic factors. Common causes include: 1. Stress and Anxiety One of the most frequent triggers, stress often manifests physically through jaw clenching or teeth grinding, particularly during sleep. 2. Sleep Disorders Conditions like sleep apnea, snoring, or insomnia are commonly linked with nighttime bruxism. 3. Misaligned Bite When the teeth don’t line up correctly (malocclusion), it may lead to unintentional grinding. 4. Medications and Substances Certain antidepressants, stimulants, caffeine, tobacco, and alcohol can increase the risk of bruxism. 5. Neurological Conditions In some cases, bruxism may be related to disorders such as Parkinson’s disease or ADHD. Determining the root cause is crucial for choosing effective bruxism treatments that provide lasting results. Common Symptoms of Bruxism Bruxism may develop silently over time. Recognizing the signs early can prevent permanent damage. Common symptoms include: Audible teeth grinding during sleep Flattened, chipped, or loose teeth Tooth sensitivity Tight or sore jaw muscles Clicking or popping sounds in the jaw Tension headaches Ear aches not caused by infection Sleep disturbances or daytime fatigue If any of these symptoms sound familiar, it’s time to explore bruxism treatments before more serious issues arise. Diagnosis: How Is Bruxism Identified? Dentists typically diagnose bruxism during routine dental exams. They look for telltale signs such as worn enamel, broken teeth, and jaw tenderness. In some cases, the following may be recommended: Dental X-rays to assess internal damage Sleep studies (polysomnography) to evaluate sleep bruxism and related disorders Patient questionnaires about stress levels, sleep quality, and lifestyle habitsAn accurate diagnosis ensures the most effective treatment plan is implemented. Professional Bruxism Treatments While lifestyle changes can help manage minor cases of bruxism, moderate to severe conditions often require professional intervention. Here are the most common clinical bruxism treatments: 1. Custom Night Guards A custom-fitted night guard (also called an occlusal splint) is one of the most effective ways to protect teeth during sleep. These devices cushion the teeth, preventing contact and reducing strain on the jaw muscles. Benefits: Prevents tooth damage Reduces jaw pain and muscle tension Improves sleep quality 2. Dental Corrections In cases where bruxism is caused by bite misalignment or missing teeth, dental treatments may include: Orthodontic work (braces or aligners) Crowns or reshaping of teeth Restorative procedures to rebuild damaged teeth Correcting the bite can eliminate the mechanical causes of grinding. 3. Botox Injections Botox is increasingly being used as a treatment for bruxism. When injected into the jaw muscles (masseter), Botox temporarily weakens them, reducing involuntary grinding and clenching. Benefits: Minimizes pain and headaches Protects teeth from wear Typically lasts 3-6 months per treatment 4. Physical Therapy Physical therapy for bruxism focuses on jaw relaxation techniques, muscle strengthening, and posture correction. Manual therapy and ultrasound treatments may also be used to reduce inflammation and improve jaw function. 5. Treatment for Sleep Disorders If bruxism is linked to sleep apnea or another disorder, treating the root sleep issue can resolve the grinding. CPAP machines, oral appliances, or behavioral therapy may be recommended. Holistic and At-Home Bruxism Treatments While professional care is vital for moderate to severe cases, certain lifestyle modifications and home remedies can greatly reduce bruxism symptoms or prevent its onset. 1. Stress Management Stress is one of the most common contributors to bruxism. Adopting effective stress reduction strategies can make a significant difference. Techniques include: Meditation and mindfulness Breathing exercises Yoga or tai chi Journaling Talking with a therapist Reducing stress helps calm the central nervous system and reduces unconscious clenching. 2. Jaw Exercises and Relaxation Stretching and relaxing the jaw muscles can ease tension and improve range of motion. Try this daily routine: Gently massage your jaw and temples Open your mouth wide and hold for a few seconds Move your jaw from side to side slowly Practice gentle breathing while resting your tongue on the roof of your mouth
Tartar Removal: A Healthy Smile Starts Here

Main Takeaways: Tartar is hardened plaque that forms quickly and can only be removed by a dental professional—not by brushing or flossing. Tartar buildup can lead to serious oral and systemic health issues, including gum disease, tooth decay, bad breath, and increased risk of heart disease and diabetes. Professional cleanings, including scaling and root planing, are essential for removing tartar and maintaining gum health. Prevention starts at home with daily brushing, flossing, a balanced diet, and avoiding sugary, sticky foods. Lifestyle habits like smoking accelerate tartar formation and interfere with healing—quitting greatly improves oral health. Children and dental implants are also vulnerable to tartar buildup, so consistent care is necessary across all age groups and dental conditions. Regular dental visits (every 6 months or as needed) and choosing an experienced provider like ADHP – Fallbrook are key to long-term oral health. Maintaining a radiant, healthy smile goes beyond just brushing and flossing. One of the most overlooked yet essential components of oral hygiene is tartar removal. Tartar, also known as dental calculus, is a hardened form of plaque that adheres stubbornly to teeth and can lead to serious dental issues if left untreated. Understanding how tartar forms, the dangers it poses, and how to remove and prevent it is crucial for anyone aiming to preserve their oral health long-term. Explore everything you need to know about tartar removal. From professional treatments and at-home prevention to the long-term effects of ignoring buildup. Let’s dive in and uncover the secrets to maintaining a cleaner, healthier smile. What Is Tartar and How Does It Form? Tartar is the calcified version of plaque—a sticky film composed of bacteria, food particles, and saliva. When plaque isn’t removed through proper brushing and flossing, it hardens within 24 to 72 hours and becomes tartar. Once formed, tartar cannot be removed by brushing alone and requires professional dental tools for complete removal. It typically accumulates along the gumline, between teeth, and in hard-to-reach areas of the mouth. The rough surface of tartar makes it easier for more plaque to accumulate, creating a vicious cycle that increases your risk for tooth decay, gum disease, and even systemic health problems. Why Tartar Removal Is So Important Tartar doesn’t just affect the appearance of your teeth—it poses serious threats to your oral and overall health. Here are some key reasons why tartar removal is crucial: Prevents Gum Disease: Tartar buildup irritates and inflames the gums, potentially leading to gingivitis or the more severe periodontitis. Reduces Bad Breath: Bacteria trapped in tartar can emit foul-smelling compounds. Protects Tooth Enamel: Tartar harbors acids that can erode enamel and lead to cavities. Improves Aesthetics: Tartar can appear yellow or brown, affecting the appearance of your smile. Minimizes Risk of Systemic Conditions: Poor oral health has been linked to heart disease, diabetes, and respiratory infections. By making tartar removal a priority, you protect more than just your teeth—you’re investing in your total body health. Professional Tartar Removal: What to Expect at the Dentist Once tartar has formed, only a dental professional can remove it effectively. During a dental cleaning, your hygienist uses specialized instruments to gently scrape away tartar from above and below the gumline. Scaling and Root Planing For more extensive buildup, especially beneath the gums, a deeper cleaning procedure known as scaling and root planing may be recommended. This involves: Scaling: Removing tartar from the surface of teeth and under the gumline. Root Planing: Smoothing the tooth roots to prevent future plaque adhesion. This method not only removes existing tartar but also helps reduce inflammation and allows the gums to reattach to the teeth. Can You Remove Tartar at Home? While brushing and flossing can prevent tartar from forming, they cannot eliminate it once it has hardened. However, certain products and habits can help slow down or minimize buildup. Dental Tools for At-Home Maintenance Some over-the-counter dental kits include scraping tools or tartar-control toothpastes. These can be helpful when used correctly, but improper use can damage enamel or gums. Always consult your dentist before attempting at-home scraping. Natural Remedies A few natural substances are believed to help reduce plaque before it hardens: Baking soda: Neutralizes acids and provides mild abrasion. Hydrogen peroxide: Helps reduce bacteria when diluted and used as a rinse. Oil pulling: Swishing coconut or sesame oil may reduce oral bacteria, though it doesn’t remove tartar. These methods can support your dental care routine, but they are not substitutes for professional tartar removal. The Role of Diet in Tartar Prevention What you eat plays a significant role in your oral health. Some foods encourage plaque formation, while others can help fight it. Foods That Promote Tartar Buildup Sugary snacks and drinks Refined carbohydrates (like white bread and chips) Sticky foods that cling to teeth Foods That Help Fight Plaque Crunchy fruits and vegetables (like apples and carrots) Cheese and yogurt (rich in calcium and phosphate) Green tea (contains antioxidants that reduce inflammation and bacteria) Incorporating more tooth-friendly foods into your diet can support your body’s natural defenses against plaque and tartar. How Smoking Affects Tartar Formation Tobacco use is one of the leading risk factors for excessive tartar buildup. Smoking decreases saliva production and promotes the growth of harmful bacteria in the mouth. This combination accelerates plaque and tartar development and also interferes with healing after tartar removal procedures. Quitting smoking not only enhances the appearance of your teeth but also greatly improves your chances of maintaining long-term oral health. How Often Should You Get Tartar Removed? For most individuals, dental cleanings every six months are sufficient to manage tartar. However, some may require more frequent visits, especially if they: Smoke Have braces or retainers Suffer from chronic gum disease Experience excessive plaque buildup Your dentist will recommend the ideal frequency based on your oral health status. Regular appointments ensure tartar is addressed before it leads to serious complications. Tartar vs. Plaque: What’s the Difference? Although often used interchangeably, plaque and tartar are not the same: Plaque is a soft,
Dental Implants in Torrance, CA
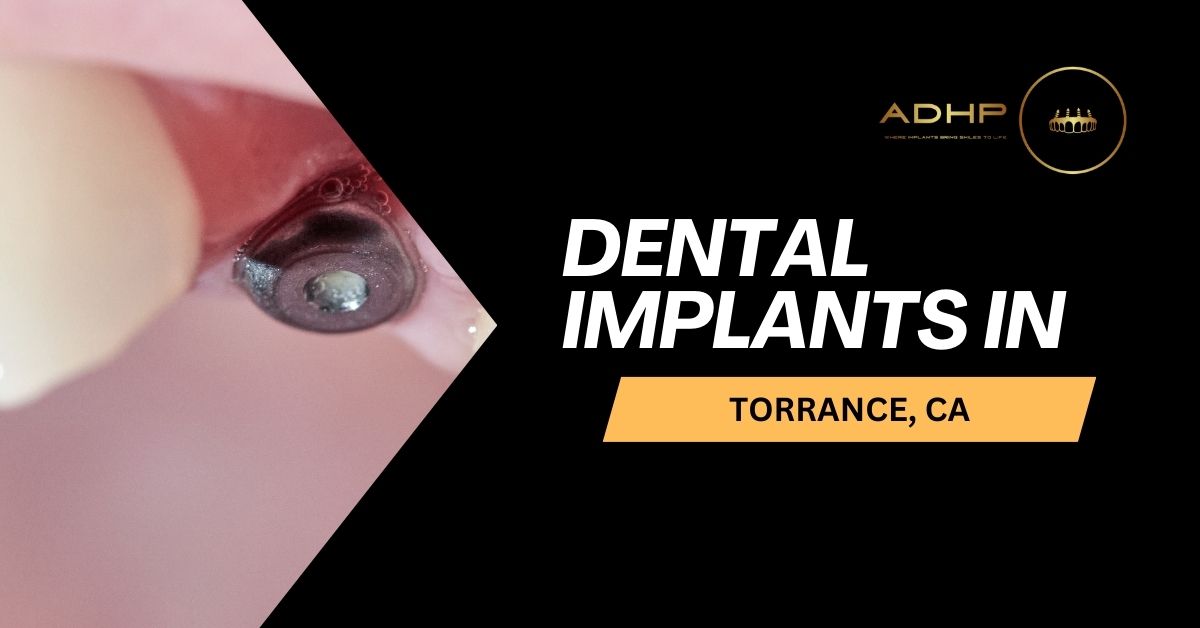
Missing teeth can have a serious impact on both your smile and your overall oral health. Whether due to injury, decay, or age, the loss of even one tooth can cause bone loss, shifting of surrounding teeth, and a drop in self-confidence. Thankfully, dental implants offer a long-lasting, natural-looking solution for replacing missing teeth. If you’re exploring dental implants Torrance CA, this comprehensive guide will help you understand the procedure, benefits, and what to expect — and why ADHP Torrance is a leading choice for implant dentistry. What Are Dental Implants? Dental implants are artificial tooth roots made from biocompatible materials like titanium. These implants are surgically placed into the jawbone where they fuse with the bone over time through a process called osseointegration. Once healed, a custom-made crown is attached to the implant, completing the restoration and delivering the look and function of a natural tooth. Unlike dentures or bridges, dental implants are designed to be permanent, offering unmatched stability and durability. Benefits of Dental Implants Dental implants are widely considered the gold standard for tooth replacement, and for good reason. Here are some of the top benefits: 1. Natural Appearance and Function Implants look, feel, and function like your natural teeth. You can eat, speak, and smile with confidence without worrying about slipping or clicking. 2. Bone Preservation When a tooth is lost, the jawbone underneath begins to deteriorate. Dental implants stimulate the bone just like natural teeth, helping to preserve bone density and facial structure. 3. Long-Term Solution With proper care, dental implants can last 20 years or longer. They offer a better return on investment over time compared to other restorations that may need to be replaced more frequently. 4. Improved Oral Health Unlike bridges that require altering adjacent teeth, implants stand alone. This helps preserve the integrity of your natural teeth and simplifies oral hygiene routines. Are You a Candidate for Dental Implants? If you’re considering dental implants Torrance CA, the first step is to determine whether you’re a good candidate for the procedure. Ideal candidates typically have: One or more missing teeth Healthy gums free from periodontal disease Adequate jawbone density to support the implant Good overall health and no uncontrolled chronic conditions Even if you’ve been told in the past that implants aren’t an option, advances in bone grafting and implant technology may change that. It’s worth consulting a specialist to explore your options. The Dental Implant Process: What to Expect Getting dental implants is a multi-step process that takes place over several months. Here’s a general overview of what to expect: 1. Consultation and Imaging During your initial visit, the implant specialist will perform a thorough examination, take X-rays or 3D scans, and develop a customized treatment plan. 2. Implant Placement The implant is surgically inserted into the jawbone under local anesthesia or sedation. After placement, the healing process can take 3 to 6 months as the implant integrates with the bone. 3. Abutment Placement Once the implant is securely fused, a small connector piece called an abutment is attached to it. This will hold the final crown in place. 4. Crown Placement Finally, a custom-made dental crown is attached to the abutment, completing your new smile. Dental Implants vs. Other Tooth Replacement Options To fully appreciate the value of dental implants Torrance CA, it helps to compare them with other common alternatives: Dentures Less expensive upfront Prone to slipping and discomfort Require adhesives May cause bone loss over time Dental Bridges Fixed in place and more stable than dentures Requires altering healthy adjacent teeth May not last as long as implants Does not prevent bone loss in the missing tooth area Implants Most natural and permanent solution Preserve bone and adjacent teeth Higher upfront cost but better long-term value When you factor in comfort, function, aesthetics, and long-term health benefits, implants are often the most effective solution. Cost of Dental Implants in Torrance, CA The cost of dental implants Torrance CA can vary depending on several factors, including: Number of implants needed Complexity of the case Need for bone grafting or sinus lifts Type of restoration (single crown, bridge, full arch) Dentist’s expertise and location On average, a single dental implant in the U.S. can range from $3,000 to $5,000. While the initial cost may seem high, implants tend to save money over time by reducing the need for replacements and additional dental work. Some insurance plans may cover a portion of the procedure, especially if it’s deemed medically necessary. Many Torrance dental offices also offer financing options or payment plans to make the procedure more accessible. How to Choose the Right Implant Dentist in Torrance Not all dental professionals are equally qualified to perform implant surgery. When choosing a provider for dental implants Torrance CA, consider the following: Experience and Credentials Look for a dentist who specializes in implant dentistry and has extensive training, preferably from organizations like the American Academy of Implant Dentistry (AAID) or the International Congress of Oral Implantologists (ICOI). Technology and Equipment Advanced diagnostic tools like 3D imaging and digital planning systems lead to more precise and successful outcomes. Patient Reviews Check online reviews and testimonials to gauge patient satisfaction and overall experience. Customized Care Choose a practice that takes the time to explain your options, listens to your concerns, and provides a tailored treatment plan that aligns with your goals. Post-Implant Care and Maintenance After receiving dental implants, proper care is crucial to ensure long-term success. Fortunately, maintenance is quite similar to caring for natural teeth: Brush twice daily with a soft-bristled toothbrush Floss daily or use an interdental brush Visit your dentist regularly for cleanings and check-ups Avoid smoking, which can interfere with healing Protect your implants from grinding or clenching (a nightguard may be recommended) With good oral hygiene and regular dental visits, your implants can serve you well for decades. Why Choose ADHP for Dental Implants in Torrance, CA? If you’re searching for dental implants Torrance CA, ADHP Torrance offers
Can Wisdom Teeth Cause Gum Recession? Understanding the Connection

Wisdom teeth, also known as third molars, often spark a number of oral health concerns as they begin to emerge in late adolescence or early adulthood. From overcrowding to infection, the complications surrounding these molars are well-documented. However, one question many patients ask their dentists is: can wisdom teeth cause gum recession? The short answer is yes, but the issue is more complex and involves various factors that intertwine oral hygiene, jaw structure, and the position of the teeth themselves. Let’s look into the connection between wisdom teeth and gum recession, identify the warning signs, and discuss available treatment options. We’ll also cover preventative measures to help you maintain a healthy smile—and why consulting with a dental expert like ADHP – Fallbrook can make all the difference. What Is Gum Recession? Before we dive into the connection, it’s essential to understand what gum recession is. Gum recession occurs when the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or its root. This can lead to increased sensitivity, higher risk of decay, and even tooth loss if left untreated. Gum recession isn’t always immediately noticeable. Some of the early signs include: Increased tooth sensitivity Visibly longer teeth Discomfort near the gumline Swollen or inflamed gums Bleeding after brushing or flossing The causes of gum recession can range from poor oral hygiene to aggressive brushing, periodontal disease, tobacco use, and genetic predisposition. But one commonly overlooked cause is the impact of wisdom teeth. How Can Wisdom Teeth Cause Gum Recession? So, can wisdom teeth cause gum recession? Absolutely. Wisdom teeth can contribute to gum recession in several ways, especially when they are impacted, partially erupted, or growing at awkward angles. 1. Impacted Wisdom Teeth and Pressure on Adjacent Teeth Impacted wisdom teeth don’t fully break through the gum line, often because they don’t have enough room to emerge. This condition can create pressure on the surrounding molars. As the pressure builds, it can disrupt the alignment of your teeth and cause the gums to recede, especially around the second molars. 2. Increased Inflammation and Infection Risk When wisdom teeth are partially erupted, they create a flap of gum tissue that traps food and bacteria. This area is incredibly difficult to clean and becomes a breeding ground for infection. The resulting inflammation can damage the surrounding gum tissue and lead to recession if not treated promptly. 3. Misalignment and Gum Trauma Wisdom teeth that grow at an angle may push against neighboring teeth. This pressure doesn’t just affect tooth alignment—it also strains the gum tissue, making it more likely to recede due to constant friction or trauma. 4. Periodontal Pockets Near Wisdom Teeth The space around erupting wisdom teeth can form what’s known as a periodontal pocket—a gap that allows bacteria to accumulate and degrade the supporting gum tissue and bone. If this pocket isn’t cleaned or treated, it can evolve into a serious infection and contribute to receding gums. Signs That Wisdom Teeth May Be Affecting Your Gums Identifying potential problems early is critical to preserving your oral health. Here are some signs that your wisdom teeth may be contributing to gum recession: Persistent bad breath or bad taste in the mouth Swelling in the back of the mouth or jaw Pain or discomfort when chewing Bleeding or tender gums near the wisdom teeth Difficulty opening your mouth fully Noticeable gum recession around nearby teeth If you’re experiencing any of these symptoms, it’s best to schedule a consultation with a dental professional. They can evaluate whether your wisdom teeth are the root cause of your gum issues. Preventative Measures to Avoid Gum Recession from Wisdom Teeth The best way to address gum recession caused by wisdom teeth is to prevent it before it starts. Here are a few proactive steps to consider: Regular Dental Check-Ups Routine dental exams allow your dentist to monitor the growth and positioning of your wisdom teeth through X-rays. Early detection of alignment issues or impaction can help prevent gum recession before it begins. Improved Oral Hygiene Keeping the back of your mouth clean is crucial. Because wisdom teeth are difficult to reach, they are more susceptible to plaque buildup. Use a soft-bristled toothbrush, floss daily, and consider a water flosser to remove debris around those hard-to-reach areas. Timely Removal of Wisdom Teeth In many cases, dentists recommend removing wisdom teeth before they can cause problems. If there’s a high risk that they’ll damage adjacent teeth or contribute to gum recession, preemptive extraction may be the best course of action. Avoiding Tobacco Products Smoking and chewing tobacco weaken the gums and make it harder for the mouth to fight off infection. Quitting these habits can significantly reduce your risk of both gum disease and gum recession. Treatment Options for Gum Recession If gum recession has already occurred—whether due to wisdom teeth or other causes—it’s important to explore treatment options. Depending on the severity, your dentist may recommend one or more of the following: Scaling and Root Planing This deep-cleaning technique removes plaque and tartar from below the gum line, helping to reduce inflammation and promote healing in mild to moderate cases of recession. Gum Graft Surgery For more severe cases, a gum graft may be necessary. This procedure involves taking tissue from another part of the mouth and attaching it to the affected area to cover exposed roots and strengthen the gum line. Antibiotic Therapy If infection is present, your dentist may prescribe antibiotics to kill the bacteria and reduce inflammation. This is often used alongside other treatments. Wisdom Tooth Extraction If wisdom teeth are found to be the root cause of gum issues, their removal can prevent further damage and support gum tissue recovery. Post-extraction care is essential to ensure proper healing and prevent additional complications. Receding Gums After Wisdom Tooth Extraction While wisdom tooth removal often prevents future gum issues, some patients may notice gum recession near the extraction site afterward. This can occur if the surrounding gum
Flexible Partial Dentures: New Dental Prosthetics

When it comes to replacing missing teeth, the options available to patients have evolved significantly over the years. One such innovative solution is flexible partial dentures. These dentures are designed to provide a comfortable, functional, and aesthetically pleasing solution for individuals who need partial tooth replacements. Whether you’re struggling with traditional dentures or looking for a more discreet option, flexible partial dentures may be exactly what you need. We’ll learn all about flexible partial dentures. From their benefits and materials to how they compare with traditional options, we aim to give you a comprehensive understanding of this groundbreaking dental solution. > What Are Flexible Partial Dentures? Flexible partial dentures are a type of dental prosthesis used to replace one or more missing teeth in the upper or lower jaw. Unlike traditional partial dentures that use metal clasps to hold them in place, flexible partial dentures are made from a flexible, thermoplastic material that allows them to adapt better to the contours of your mouth. This unique flexibility makes them more comfortable and natural-looking compared to conventional dentures. These dentures are typically used when a patient has several missing teeth but still has some natural teeth remaining. They fill in the gaps, restore the ability to chew and speak, and enhance the appearance of the smile. Most importantly, flexible partial dentures offer a far less noticeable solution than traditional, rigid dentures. The Materials Used in Flexible Partial Dentures One of the most distinctive aspects of flexible partial dentures is the material from which they are made. The most common materials used for these dentures include: 1. Nylon-Based Materials Nylon is one of the primary materials used in the creation of flexible partial dentures. This material is known for its flexibility and durability. It’s also incredibly lightweight, which ensures that the dentures don’t feel bulky or uncomfortable in the mouth. 2. Valplast Valplast is a widely used thermoplastic resin specifically designed for flexible partial dentures. It’s a biocompatible material that adapts easily to the contours of your mouth. Valplast is highly durable, resistant to wear, and offers a smooth, natural appearance that blends seamlessly with your natural teeth. 3. Kraton Kraton is another popular thermoplastic material used in flexible partial dentures. It offers a high degree of elasticity and is resistant to cracking, making it a long-lasting solution for partial dentures. 4. Tritan Tritan is a newer material that is highly flexible, lightweight, and durable. It’s often used for people who require more comfortable dentures that adapt quickly to the shape of their mouth. Each of these materials has its advantages, but they all share one common feature: they are designed to provide a more natural, comfortable fit compared to traditional partial dentures. Benefits of Flexible Partial Dentures Flexible partial dentures offer a variety of benefits over traditional dentures. Here are some of the key advantages: 1. Improved Comfort Traditional dentures can be uncomfortable because they are rigid and often don’t fit well in the mouth. Flexible partial dentures, on the other hand, mold better to the shape of your gums, reducing irritation and discomfort. Their lightweight construction ensures they don’t feel bulky or heavy. 2. Aesthetically Pleasing One of the most significant benefits of flexible partial dentures is their ability to blend in seamlessly with your natural teeth and gums. The flexible material is often transparent or matches the color of your gum tissue, making the dentures less noticeable compared to the metal clasps and visible acrylic of traditional dentures. 3. Durability and Longevity Flexible dentures are built to last. The materials used, such as Valplast and Kraton, are highly resistant to cracks and fractures, offering a more durable solution. These dentures can withstand normal wear and tear and maintain their functionality and appearance for a long time. 4. Less Maintenance Unlike traditional dentures that may require adjustments, flexible partial dentures are often easier to maintain. They don’t need the same level of upkeep, such as frequent relining or repair, as they fit snugly in place from the beginning. 5. More Natural Fit Flexible partial dentures are custom-designed to fit the unique shape of your mouth. Because of the flexibility of the materials, they can adapt more closely to your gums and remaining teeth, providing a more natural feel and better retention. 6. No Need for Metal Clasps The absence of metal clasps is one of the standout features of flexible partial dentures. Instead, the flexible material itself helps the denture stay securely in place. This offers not only a more comfortable fit but also a more aesthetically pleasing result. Flexible Dentures for Patients with Allergies or Sensitivities Flexible dentures are an ideal solution for individuals who experience allergies or sensitivities to traditional dental materials. Many conventional dentures include metal components or acrylics that can cause irritation or allergic reactions. Flexible dentures, however, are crafted from hypoallergenic materials like nylon or thermoplastic resin, which are gentle on the gums and oral tissues. This makes them especially suitable for patients with sensitive mouths or known material sensitivities. By eliminating common allergens, flexible dentures provide a comfortable and safe alternative that allows wearers to enjoy improved function and aesthetics without the risk of discomfort or irritation. How Do Flexible Partial Dentures Compare to Traditional Dentures? Traditional dentures have been around for many years and are still widely used to replace missing teeth. However, they have several limitations that flexible partial dentures help overcome. Here’s how they compare: Comfort and Fit Traditional dentures can often feel bulky and uncomfortable because they don’t conform to the natural shape of your mouth. Flexible partial dentures, by contrast, are made of a more pliable material that molds better to the contours of your gums, leading to a more comfortable experience overall. Aesthetic Appeal Traditional dentures, especially partial dentures, may involve visible metal clasps or bulky acrylic. Flexible partial dentures look far more natural because they are made from translucent or gum-colored materials that blend in with your mouth. The absence of metal clasps contributes to their
Choosing the Best Dental Implant Cleaner
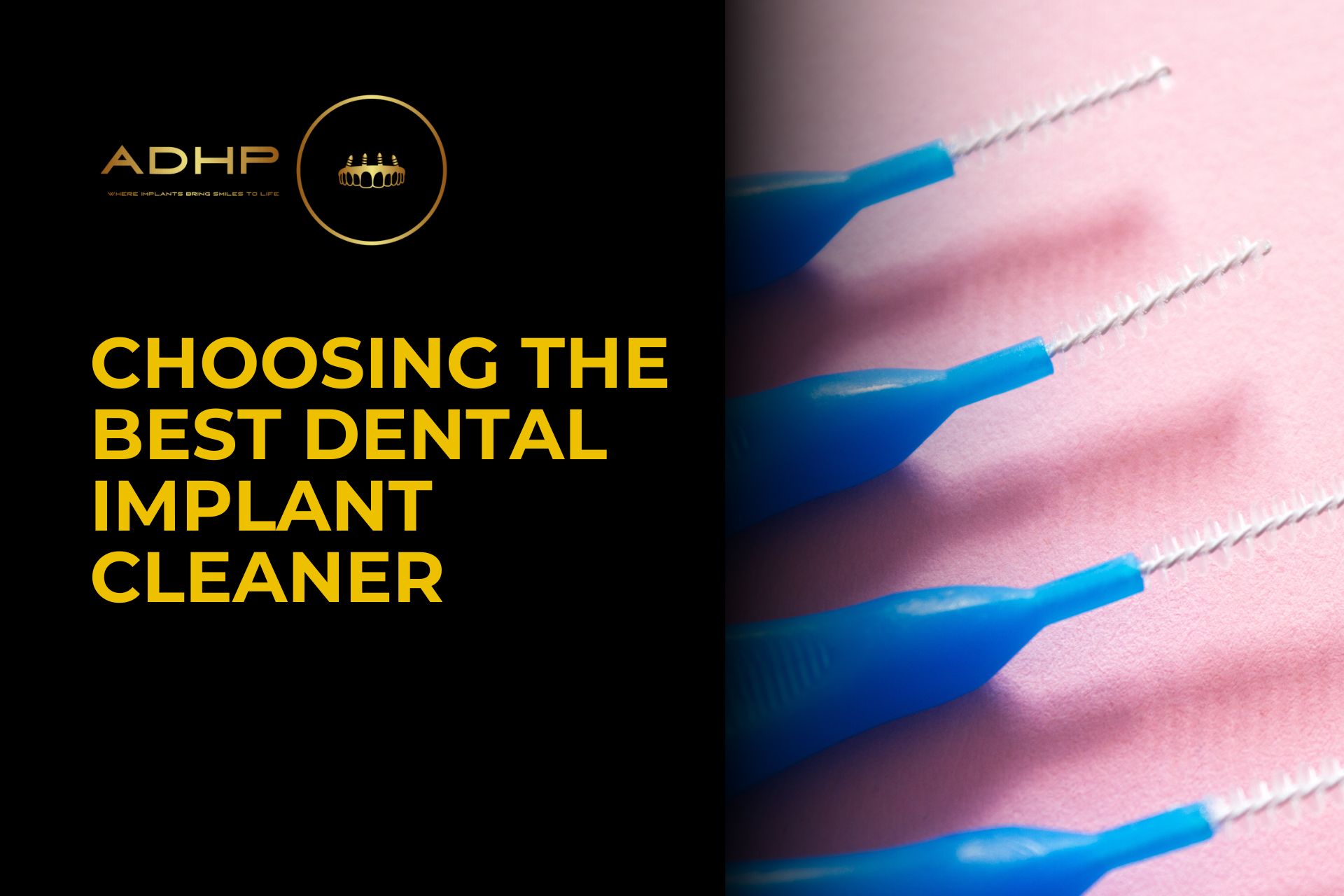
Dental implants are a significant investment in your oral health and overall well-being. To protect that investment, proper care is essential. One of the most important tools in maintaining your dental implants is a high-quality dental implant cleaner. In this guide, we will explore the best ways to clean dental implants, the importance of specialized cleaning products, and expert tips for keeping your smile healthy and radiant. Why Cleaning Dental Implants Matters Dental implants mimic the function and appearance of natural teeth. However, unlike natural teeth, they require meticulous care to prevent complications such as gum disease, peri-implantitis, and plaque buildup. Using a suitable dental implant cleaner ensures that your implants remain free of harmful bacteria and stay in excellent condition for years to come. What is a Dental Implant Cleaner? A dental implant cleaner is a specialized tool or product designed to help maintain the cleanliness and health of dental implants. These cleaners can come in various forms, including: Interdental Brushes: Perfect for cleaning hard-to-reach areas around implants. Water Flossers: Use water pressure to dislodge plaque and debris. Implant-Safe Toothpaste: Formulated to be gentle on implant surfaces. Antimicrobial Mouthwash: Helps control bacteria around the implants. Choosing the right dental implant cleaner depends on your specific needs and oral care routine. Features to Look for in a Dental Implant Cleaner When selecting a dental implant cleaner, consider the following features: Gentleness: Ensure the product is safe for both your implants and surrounding gum tissue. Effectiveness: Look for products that effectively remove plaque and bacteria. Ease of Use: Cleaning tools should be user-friendly and convenient. Compatibility: Ensure the cleaner works well with both implants and natural teeth. Types of Dental Implant Cleaners 1. Interdental Brushes Interdental brushes are small brushes designed to clean between teeth and around implants. They are ideal for reaching tight spaces that regular toothbrushes can’t access. Look for brushes with soft, flexible bristles. Choose the appropriate size for your gaps. Use gentle back-and-forth motions to clean around implants. 2. Water Flossers Water flossers, also known as oral irrigators, are highly effective for cleaning dental implants. Use a water flosser with adjustable pressure settings. Direct the water stream at the gumline and around each implant. Look for models with specialized tips for implant care. 3. Soft-Bristled Toothbrushes A soft-bristled toothbrush is gentle enough for cleaning implants while effectively removing plaque. Use a brush with rounded bristles. Brush in gentle circular motions. Avoid hard-bristled brushes that can damage gums and implant surfaces. 4. Implant-Safe Toothpaste Not all toothpaste is suitable for dental implants. Some abrasive formulas can scratch implant surfaces. Look for non-abrasive toothpaste. Choose fluoride-free options if recommended by your dentist. Opt for toothpaste with antibacterial properties. 5. Antimicrobial Mouthwash Rinsing with antimicrobial mouthwash helps control bacteria and freshen your breath. Choose alcohol-free mouthwash to avoid irritation. Swish the mouthwash for at least 30 seconds. Use mouthwash as a supplement, not a replacement for brushing and flossing. Best Practices for Cleaning Dental Implants To maintain your dental implants, follow these expert tips: Brush Twice Daily: Use a soft-bristled toothbrush to clean implants and natural teeth. Floss Regularly: Consider water flossers or specialized floss for implants. Use Antimicrobial Products: Control bacteria with mouthwash and implant-safe solutions. Schedule Professional Cleanings: Visit your dentist every six months or as recommended. Inspect Implants: Regularly check for signs of inflammation or damage. Common Mistakes to Avoid Using Abrasive Cleaners: Harsh toothpaste or brushes can damage implants. Neglecting Gum Health: Healthy gums are essential for implant longevity. Skipping Regular Dental Visits: Professional cleanings help maintain implant health. Improper Flossing: Avoid snapping floss against the gumline, which can cause irritation. Best Toothbrush for Dental Implants Not all toothbrushes are equally effective for dental implants. A soft-bristled toothbrush is highly recommended, as it gently cleans without scratching the implant surface or irritating your gums. For those who prefer advanced options, an electric toothbrush with pressure control offers added benefits. Its consistent motion, built-in timer, and pressure sensor ensure a thorough clean while preventing excessive force that could harm the gum line around your implants. Best Mouthwash for Dental Implants The right mouthwash plays an important role in maintaining implant health. An alcohol-free antimicrobial rinse is the safest choice, as it helps control bacteria without drying out or irritating sensitive tissues. Alcohol-based rinses, on the other hand, may cause gum irritation and compromise healing around implants. Look for formulas specifically designed for implants or sensitive gums, which provide effective protection while keeping your breath fresh and your implants strong. Signs You Need to Improve Your Dental Implant Care Persistent bad breath Red, swollen, or bleeding gums Loose implants Pain or discomfort around the implant site If you notice any of these signs, consult your dentist and evaluate your dental implant cleaning routine. Benefits of Proper Dental Implant Care Maintaining a diligent cleaning routine with the right dental implant cleaner offers numerous benefits: Enhanced Implant Longevity: Proper care helps implants last for decades. Healthier Gums: Prevents gum disease and inflammation. Improved Oral Hygiene: Reduces plaque and bacteria buildup. Better Aesthetics: Keeps your smile bright and beautiful. Expert Tips for Maintaining Dental Implant Health Create a Consistent Oral Hygiene Routine: Establish a daily schedule that includes brushing, flossing, and rinsing. Consistency is key to preventing plaque buildup and bacterial growth. Use Dental Tools Designed for Implants: Standard toothbrushes and floss may not be enough. Consider investing in tools specifically designed for cleaning around dental implants. Stay Hydrated: Drinking plenty of water helps rinse away food particles and bacteria. Staying hydrated also promotes healthy saliva production, which naturally protects your mouth. Monitor Your Diet: Avoid sticky, sugary foods that can contribute to plaque formation. Opt for a balanced diet rich in fruits, vegetables, and lean proteins. Don’t Ignore Discomfort: Any pain, swelling, or irritation around your implants should be addressed promptly by a dental professional. Quit Smoking: Smoking can increase the risk of implant failure and gum disease. If you smoke, consider seeking support to quit. Follow Post-Procedure Care
Avoiding Dental Implant Scams

Dental implants are a life-changing solution for many individuals seeking to restore their smiles. However, the rise in demand has also led to an increase in fraudulent practices. Unsuspecting patients often fall prey to dental implant scams, resulting in financial loss and health complications. This guide explores how to identify and avoid these scams, providing tips to ensure you choose a trustworthy provider. What Are Dental Implant Scams? Dental implant scams are deceptive practices aimed at exploiting patients seeking dental implant procedures. These scams often involve unqualified practitioners, substandard materials, or misleading advertising. Victims may end up with poorly performed procedures that require costly corrections or, worse, suffer long-term oral health damage. Warning Signs of Dental Implant Scams Recognizing red flags is the first step in protecting yourself from scams. 1. Unbelievably Low Prices If a dental practice advertises implants at a fraction of the usual cost, it’s worth investigating. Scammers often lure patients with prices that seem too good to be true. 2. Lack of Credentials Qualified dentists should have certifications and training in implant dentistry. If these qualifications are absent or unverifiable, it’s a major warning sign. 3. Pressure to Commit Scammers often pressure patients to make hasty decisions. Genuine practices prioritize patient education and allow time for thoughtful consideration. 4. Limited Transparency If a provider is vague about the materials used or the procedure’s cost breakdown, proceed with caution. Transparency is key to a trustworthy practice. The Cost of Falling Victim to Dental Implant Scams Dental implant scams can have far-reaching consequences. 1. Financial Loss Correcting a botched implant procedure is often more expensive than having it done correctly the first time. Victims may also lose their initial investment entirely. 2. Health Risks Substandard implants or improper procedures can lead to infections, bone damage, or implant failure, necessitating additional surgeries. 3. Emotional Impact A failed implant can be emotionally devastating, especially for patients who were eager to regain their smiles. How to Choose Reputable Dental Implant Providers Avoiding dental implant scams begins with thorough research and due diligence. 1. Verify Credentials Ensure the dentist is licensed and has specialized training in implant dentistry. Memberships in professional organizations like the American Academy of Implant Dentistry are also a good sign. 2. Check Reviews and Testimonials Online reviews and patient testimonials can provide insight into the provider’s reputation. Be cautious of practices with consistently negative feedback. 3. Ask About Materials High-quality dental implants are made from biocompatible materials like titanium or zirconia. Confirm that the provider uses trusted brands. 4. Request a Consultation A reputable provider will offer a thorough consultation to discuss your needs, explain the procedure, and address your concerns. Types of Dental Implant Scams to Watch Out For Understanding common scam tactics can help you stay vigilant. 1. Bait-and-Switch Pricing Some providers advertise low prices but add hidden fees during the treatment process. Always get a detailed cost estimate upfront. 2. Unnecessary Procedures Scammers may recommend treatments you don’t need to inflate costs. Seek a second opinion if a diagnosis seems excessive. 3. Counterfeit Implants Counterfeit or low-quality implants can fail quickly, leading to complications. Insist on authentic, FDA-approved materials. 4. Fake Dental Reviews Some fraudulent practices post fake reviews to appear credible. Look for reviews on multiple platforms for a more accurate picture. Protecting Yourself from Dentist Scams Another effective way to safeguard against dental implant fraud is to verify a provider’s professional affiliations and continuing education. Reputable dentists often participate in professional organizations, attend industry conferences, and pursue ongoing training in implantology. This commitment to professional development indicates adherence to current best practices and evidence-based techniques. Additionally, checking for state board certifications and reviewing any disciplinary history can provide further assurance of credibility. By combining credential verification with patient reviews and material transparency, you can make a more informed decision and reduce the risk of falling victim to implant scams. Taking proactive measures can save you from falling victim to scams. 1. Research Thoroughly Spend time researching potential providers. Verify their credentials, experience, and patient satisfaction rates. 2. Ask Questions Don’t hesitate to ask about the dentist’s qualifications, the materials used, and the procedure’s details. A trustworthy provider will welcome your inquiries. 3. Trust Your Instincts If something feels off—whether it’s the pricing, the provider’s demeanor, or the clinic’s environment—it’s better to walk away. 4. Consult Multiple Providers Getting quotes and opinions from multiple providers ensures you’re making an informed decision. The Role of Dental Insurance in Preventing Scams Dental insurance can be a valuable tool in avoiding scams. 1. Vetted Providers Insurance companies often work with a network of verified dentists, reducing the risk of encountering scammers. 2. Cost Transparency Insurance plans provide clear information about coverage and out-of-pocket expenses, making it harder for scammers to inflate costs. 3. Second Opinions Many insurance plans cover second opinions, allowing you to confirm the necessity and legitimacy of a recommended procedure. The Importance of Regular Dental Checkups Regular dental checkups not only maintain oral health but also help detect potential issues early. Dentists can identify signs of failed implants or improper work, providing an opportunity for timely correction. Understanding the Dental Implant Process Educating yourself about the standard dental implant process can help you recognize irregularities. The process typically involves consultation, imaging, bone grafting if necessary, implant placement, healing time, and crown placement. If a provider skips critical steps, consider it a red flag. The Impact of Technological Advancements in Implant Dentistry Legitimate providers invest in advanced dental technology for precise implant placement. Technologies like 3D imaging and computer-guided surgery improve accuracy and outcomes. Clinics lacking modern equipment may compromise patient care. The Importance of Aftercare in Dental Implants A reputable dental provider will emphasize the importance of post-procedure care. Aftercare instructions help ensure the implant heals properly and integrates with the jawbone. Be cautious if a provider does not offer guidance on maintaining oral hygiene or follow-up visits. Common Myths About Dental Implants Misinformation can also contribute to falling victim to scams. One
How to Clean Dental Implants for Lasting Oral Health

Dental implants have transformed the way people approach tooth replacement, offering a durable, natural-looking solution. But just like natural teeth, implants require regular care to ensure they remain healthy and functional. Learning how to clean dental implants is essential to prevent complications like plaque buildup, gum disease, and implant failure. In this comprehensive guide, we’ll cover the best practices for maintaining your dental implants, from daily cleaning routines to specialized care tips, ensuring your investment in a healthier smile is protected for years to come. Why Cleaning Dental Implants is Essential Dental implants are crafted from materials like titanium and ceramic, known for their durability and compatibility with the human body. However, without proper care, implants can develop plaque and tartar buildup, leading to gum inflammation, a condition called peri-implantitis, and even implant failure. Understanding how to clean dental implants ensures their longevity and promotes a healthy mouth overall. Basic Daily Care: How to Clean Dental Implants at Home Daily cleaning is vital to maintaining healthy implants. Here’s a step-by-step guide to caring for your implants each day: 1. Brush Twice Daily Brushing your teeth twice a day is a must for everyone, but it’s especially important for those with dental implants. Use a soft-bristled toothbrush or an electric toothbrush designed for sensitive teeth to avoid damaging the implant surface or irritating surrounding gum tissue. Gently brush around the implant, ensuring you reach all sides. 2. Use a Low-Abrasive Toothpaste It’s crucial to use a non-abrasive toothpaste to prevent scratching the implant surface. Many whitening toothpastes contain abrasive agents, so it’s best to avoid these. Opt for toothpaste that is specially formulated for sensitive teeth or those recommended by your dental provider. 3. Floss Daily Around Your Implants Flossing is essential to remove food particles and plaque between teeth and around your implants. Choose unwaxed floss or a floss threader to get between tight spaces and along the gum line. Some prefer water flossers as a gentler option to reach hard-to-access areas around the implant, which may be particularly beneficial for those with multiple implants. 4. Use an Antibacterial Mouthwash Rinsing with an antibacterial mouthwash helps eliminate bacteria that brushing and flossing might miss. Choose a mouthwash that is alcohol-free to avoid drying out the gums and causing irritation. Advanced Tips on How to Clean Dental Implants While daily brushing and flossing are critical, there are additional techniques that can help keep your implants clean and gums healthy: 1. Invest in a Water Flosser for Implants Water flossers, such as Waterpik, use a stream of water to remove plaque and food particles from between teeth and around implants. They are especially useful for people with implants, as they can reach areas regular floss might miss. Using a water flosser on a low to medium setting is gentle on the gums, preventing inflammation while ensuring effective cleaning. 2. Consider Interdental Brushes Interdental brushes are small, cone-shaped brushes designed to clean between teeth and implants. Choose an interdental brush with a soft, nylon bristle that fits comfortably between your implant and natural teeth. This can be an excellent tool for removing debris without causing irritation or scratching the implant surface. 3. Try a Rubber-Tipped Stimulator A rubber-tipped stimulator is designed to massage the gums and remove plaque from hard-to-reach areas around your implants. Using this tool gently along the gum line can improve circulation and keep gums healthy. Professional Care: When to Visit Your Dentist In addition to your home care routine, regular visits to your dentist are essential for implant maintenance. Here’s what you can expect during professional cleaning appointments: 1. Routine Checkups Every Six Months Regular checkups allow your dentist to assess the health of your gums and implants. They’ll examine the implant site for signs of inflammation or bone loss and check for any early signs of peri-implantitis. These visits are crucial for maintaining the integrity of the implant over time. 2. Professional Cleanings with Special Tools Professional cleanings for dental implants differ from regular dental cleanings. Your dental hygienist will use specialized tools, like plastic or titanium-tipped scalers, which are gentle on implant surfaces. This ensures that plaque and tartar are thoroughly removed without damaging the implant. 3. X-Rays to Monitor Bone Health Your dentist may periodically take X-rays of your implant to monitor the health of the surrounding bone structure. This can help detect any early issues, such as bone loss, that could compromise the implant’s stability. Avoiding Common Mistakes When Cleaning Dental Implants Proper care of dental implants requires avoiding certain mistakes that could lead to gum irritation or implant damage. Here’s what to keep in mind: 1. Avoid Abrasive Cleaning Tools Using abrasive toothbrushes, toothpastes, or dental tools can scratch the surface of your implant, creating places for bacteria to thrive. Stick to soft-bristled brushes and non-abrasive cleaning agents. 2. Skip Hard or Sticky Foods While dental implants are designed to handle the pressures of daily chewing, hard and sticky foods can still pose a risk. Foods like hard candies, nuts, or gum can dislodge or damage the implant crown over time. Whenever possible, avoid these to protect your investment. 3. Don’t Ignore Gum Sensitivity or Bleeding If you experience bleeding gums or sensitivity around your implant, it could be an early sign of peri-implantitis or inflammation. Ignoring these signs may lead to more severe issues down the road. If you notice any changes, contact your dentist to address the problem promptly. How to Clean Dental Implants with Removable Appliances For those with implant-supported dentures or bridges, cleaning requires additional care. Removable appliances should be taken out and cleaned thoroughly each day to prevent bacteria from building up along the gum line and around the implants. 1. Remove and Brush Daily Take out the appliance and brush it gently with a soft brush. Make sure to clean around the implants and underneath the denture base to remove any trapped debris. 2. Use a Denture Cleaner for Additional Sanitation Soak your appliance in a

