Dental Implant Consultation: What to Expect and Why It Matters
Main Takeaways A dental implant consultation is a comprehensive planning session—far more than just an exam—designed to assess oral health, bone support, and individual needs before proceeding with implants. Key assessment areas include oral health, bone density, medical history, and lifestyle habits; these help determine candidacy and whether additional procedures (like bone grafting) may be necessary. Consultation steps typically include a medical/dental history review, oral exam, imaging or scans, treatment discussion (including alternatives), and a cost estimate with financing options. Advanced technology such as 3D CBCT scans, intraoral scanners, and computer-guided implant placement improve precision and treatment outcomes. Comparing options—implants vs. dentures or bridges—helps patients understand benefits like stability, longevity, and natural appearance when making informed decisions. Benefits of a thorough consultation include higher success rates, personalized treatment, clear expectations, and building trust with your dental provider. Preparation tips for patients: bring medical records, prepare questions, be honest about habits like smoking, and understand budget considerations to make the most of the appointment. For many people, missing teeth affect more than just appearance. They can change how you speak, limit what you eat, and lower your confidence. Dental implants have become one of the most trusted solutions for restoring smiles because they look, feel, and function like natural teeth. But before you can move forward with treatment, the process begins with a dental implant consultation. This important first step helps determine if implants are the right choice for you and sets the foundation for successful treatment. In this article, we’ll explore what happens during a consultation, why it’s essential, and how you can prepare for it. What Is a Dental Implant Consultation? A dental implant consultation is an in-depth appointment with a dental professional who specializes in implant dentistry. During this visit, your dentist or prosthodontist reviews your oral health, medical history, and treatment goals. It’s more than just an exam—it’s a chance to create a personalized plan that ensures your implants will last for years. Think of it as the roadmap to your new smile. Without it, treatment may not account for important details such as bone density, gum health, or underlying medical conditions. Why a Consultation Is Essential Many patients wonder why they can’t just jump straight into implant treatment. The truth is that implants require precision and planning. A consultation is important for several reasons: Assessment of Oral Health – Your dentist checks for gum disease, cavities, and other issues that must be treated first. Bone Density Evaluation – Dental implants need strong bone support. If your jawbone has weakened, a bone graft may be recommended. Customized Treatment Planning – Everyone’s mouth is unique. A consultation ensures your implants are designed to match your bite and smile. Medical Review – Certain health conditions, like uncontrolled diabetes, may affect healing. Your dentist will discuss any concerns. Expectation Setting – This is your chance to ask questions and learn what the process, recovery, and results will look like. Without this step, implants could fail or not meet your expectations. The Steps of a Dental Implant Consultation When you schedule your consultation, here’s what you can expect during your appointment: 1. Medical and Dental History Review Your dentist will ask about medications, chronic illnesses, and previous dental work. This helps identify potential risks and tailor the treatment. 2. Comprehensive Oral Exam Your teeth, gums, and bite are evaluated to determine if your mouth is healthy enough for implants. 3. Imaging and Scans X-rays or 3D scans provide a detailed look at your jawbone and surrounding structures. These images are critical for precise implant placement. 4. Discussion of Treatment Options Your dentist will explain whether implants are the best choice or if alternative treatments, like bridges or dentures, may be better. 5. Cost Estimate and Financing Options You’ll receive a breakdown of fees, insurance coverage, and financing options if available. Questions to Ask During Your Consultation A dental implant consultation is a two-way conversation. It’s important to feel comfortable and informed before making a decision. Here are some smart questions to ask: How many dental implant procedures have you performed? Am I a good candidate for implants? What type of implant system do you use? How long does the process take from start to finish? What are the risks and potential complications? What financing or payment plans are available? Asking these questions helps you feel confident about your treatment and the expertise of your provider. Who Is a Candidate for Dental Implants? Not everyone qualifies for implants right away. Candidates usually meet these criteria: Good overall oral health and no active gum disease. Sufficient jawbone density to support the implant. Non-smokers, or willingness to stop smoking during healing. No uncontrolled medical conditions that interfere with recovery. If you don’t meet all requirements, don’t worry. Procedures like bone grafts, sinus lifts, and periodontal treatments can improve eligibility. The Role of Technology in Consultations Modern dental technology has made consultations far more precise than in the past. Some tools commonly used include: Cone Beam CT Scans: 3D imaging that shows jawbone quality and nerve locations. Intraoral Scanners: Digital impressions that replace messy molds. Computer-Guided Implant Placement: Software that maps the exact location for implant posts. These advancements improve accuracy, reduce risks, and shorten recovery times. Comparing Implants to Other Tooth Replacement Options During your consultation, your dentist may explain alternatives to implants. Here’s how implants compare: Dentures: Less expensive but less stable; may slip or cause discomfort. Bridges: Fixed solution but may require reshaping healthy teeth. Implants: Permanent, stable, and the closest match to natural teeth. Understanding the pros and cons ensures you make the right choice for your lifestyle and budget. Benefits of a Thorough Consultation Taking the time for a full dental implant consultation offers long-term advantages: Higher Success Rate – Careful planning reduces complications. Personalized Results – Implants are customized to your bite and facial structure. Peace of Mind – You know what to expect at every stage of treatment. Stronger Patient-Doctor Relationship – The consultation builds trust and
What Is a Prosthodontist?
Main Takeaways: Prosthodontics is a dental specialty focused on restoring and replacing teeth, supporting oral function, comfort, and aesthetics. A prosthodontist undergoes three additional years of specialized training beyond dental school Prosthodontists excel in complex dental cases, including implants, crowns, bridges, dentures, veneers, and full-mouth rehabilitation—using precision and customization to achieve natural-looking results They are often referred to as the “architects of the smile,” blending dental science with artistry to create harmony between teeth, gums, and facial structure Advanced technology and techniques set prosthodontists apart—from CAD/CAM same-day restorations and 3D printing, to digital smile design and use of durable materials like zirconia Ideal patients for prosthodontic care include those with missing or severely damaged teeth, TMJ disorders, jaw pain, congenital or trauma-related dental issues, or needing a complex, cosmetic smile makeover They often work in coordination with oral surgeons, orthodontists, periodontists, and general dentists to provide holistic treatment that addresses both functional and aesthetic goals Choosing a prosthodontist ensures precision, aesthetics, durability, and comprehensive care—restoring oral health and confidence for patients with challenging dental needs When it comes to oral health, most people are familiar with general dentists, orthodontists, and even oral surgeons. But there’s another highly specialized field in dentistry that many patients don’t know much about: prosthodontics. If you’ve ever wondered, “what is a prosthodontist?” you’re not alone. These specialists play a critical role in restoring smiles, replacing missing teeth, and rebuilding oral function. In this guide, we’ll break down exactly what prosthodontists do, how they differ from other dental professionals, the treatments they provide, and why you might need to see one. Understanding Prosthodontics Prosthodontics is a recognized dental specialty that focuses on the restoration and replacement of teeth. The word comes from “prosthesis,” meaning an artificial replacement, and “odont,” meaning tooth. A prosthodontist is essentially a dentist who has advanced training in designing, creating, and fitting dental restorations such as crowns, bridges, dentures, and dental implants. Unlike general dentists, who handle a broad range of preventive and restorative procedures, prosthodontists concentrate on complex cases that require precision, customization, and advanced knowledge of dental materials. What Is a Prosthodontist? A prosthodontist is a dentist who has completed an additional three years of specialized training after dental school. This training is accredited by the American Dental Association (ADA) and focuses on the diagnosis, treatment planning, and rehabilitation of oral function and aesthetics. In simple terms, if your dental needs go beyond fillings and cleanings, a prosthodontist is the expert who restores your smile when it’s damaged, incomplete, or missing teeth. They are sometimes called the “architects of the smile” because they don’t just treat teeth—they restore harmony between teeth, gums, and facial structure. How Prosthodontists Differ from General Dentists While both general dentists and prosthodontists care for patients’ oral health, there are key differences: Education: Prosthodontists undergo three additional years of training focused exclusively on complex restorative and cosmetic dentistry. Expertise: They specialize in rebuilding smiles, treating bite problems, and managing advanced tooth loss. Technology: Prosthodontists use advanced imaging, digital dentistry, and state-of-the-art techniques for precision outcomes. Complex Cases: They often treat patients with congenital conditions, traumatic injuries, or extensive wear caused by grinding and other issues. Think of it this way: a general dentist is like your primary care doctor, while a prosthodontist is a dental specialist you see for advanced treatment. Common Treatments Provided by Prosthodontists Prosthodontists handle a wide range of restorative and cosmetic procedures. Some of the most common include: 1. Dental Implants Prosthodontists are leaders in dental implant placement and restoration. Implants replace missing teeth with artificial roots that support crowns, bridges, or dentures. 2. Crowns and Bridges These restorations repair damaged teeth or replace missing ones. Prosthodontists ensure they fit seamlessly and look natural. 3. Dentures From complete dentures for patients missing all teeth to partial dentures for those missing just a few, prosthodontists customize prosthetics for comfort and function. 4. Veneers Thin porcelain shells placed on the front of teeth to improve shape, color, and alignment. 5. Full-Mouth Rehabilitation Patients with severe damage or multiple missing teeth may require a comprehensive plan combining implants, crowns, and other restorations. 6. TMJ Disorder Treatment Prosthodontists help patients manage jaw pain and bite misalignment that affects chewing and speech. Cosmetic Dentistry and Aesthetic Expertise Prosthodontists don’t just restore function—they also enhance appearance. Because they understand the balance between teeth, gums, lips, and facial structure, they are uniquely qualified to design smiles that look natural and healthy. Treatments may include veneers, teeth whitening, reshaping, and full smile makeovers. This makes them the go-to specialists for patients who want both function and beauty in their dental restorations. Who Should See a Prosthodontist? Not every patient will need to see a prosthodontist, but certain situations make their expertise invaluable. You may benefit from visiting one if you: Are missing one or more teeth. Have severely worn or damaged teeth. Suffer from TMJ disorders or chronic jaw pain. Require a complex dental treatment plan involving multiple procedures. Want a complete smile makeover with both functional and aesthetic improvements. Have congenital dental conditions or experienced trauma that damaged your teeth. The Role of Prosthodontists in Dental Teams Prosthodontists often collaborate with other dental professionals, including: Oral surgeons (for implant placement and extractions). Periodontists (for gum treatments). Orthodontists (for tooth alignment). General dentists (for preventive and routine care). By working together, these professionals ensure patients receive comprehensive care that addresses both oral health and cosmetic goals. Prosthodontics vs. Other Dental Specialties You may be wondering how prosthodontists compare to other dental specialists. Here’s a quick breakdown: Orthodontist: Focuses on straightening teeth and correcting bites with braces or aligners. Oral Surgeon: Specializes in surgical procedures, such as extractions and implant placement. Periodontist: Focuses on gum health and supporting structures of the teeth. Prosthodontist: Specializes in restoring missing or damaged teeth and improving aesthetics. While some overlap exists, prosthodontists stand out for their expertise in complex restorative and cosmetic procedures. Benefits of Seeing a Prosthodontist Choosing a prosthodontist can provide several
Sedation Dentistry: A Comfortable Path to Better Oral Health
Main Takeaways: Sedation dentistry uses medications like nitrous oxide, oral sedatives, IV sedation, or general anesthesia to help patients relax during dental care. It is especially helpful for people with dental anxiety, sensitive teeth, strong gag reflexes, special needs, or complex treatment plans. Options include nitrous oxide for mild relaxation, oral conscious sedation for deeper calm, IV sedation for adjustable depth, and general anesthesia for full unconsciousness. Benefits include reduced anxiety, minimal discomfort, suppressed gag reflex, ability to complete multiple treatments in one visit, and little to no memory of the procedure. Sedation dentistry improves patient comfort and accessibility, making dental care possible for those who might otherwise avoid treatment. Procedures are performed under professional supervision with advanced monitoring for safety. ADHP offers sedation dentistry across multiple Southern California locations, ensuring care is accessible and stress-free. For many people, the thought of visiting the dentist brings feelings of anxiety or even fear. Whether it’s the sound of dental tools, the smell of the office, or bad past experiences, dental visits can be a source of stress. But what if you could have your dental work done while feeling calm, relaxed, and completely at ease? That’s the goal of sedation dentistry—a solution that helps patients overcome dental anxiety and get the care they need without fear or discomfort. This article will walk you through what sedation dentistry is, who it helps, the different types of sedation used, and what to expect before, during, and after your visit. We’ll also talk about safety, costs, and how it can change your relationship with oral care. What Is Sedation Dentistry? Sedation dentistry is a method used by dental professionals to help patients feel calm and comfortable during procedures. It involves using medication to help patients relax or even sleep while their dental work is being done. While you’re not always completely asleep (unless under general anesthesia), you’ll feel deeply relaxed and often won’t remember much of the procedure afterward. This type of care is especially useful for longer procedures or for patients who have a strong fear of dental visits. It allows the dentist to work more efficiently while making the experience much easier for the patient. Who Can Benefit from Sedation Dentistry? Sedation dentistry isn’t just for people with severe dental phobia. It’s helpful for a wide range of individuals, including: People with dental anxiety or fear Children or adults with special needs Those with a strong gag reflex Patients needing multiple procedures in one visit Anyone with very sensitive teeth People who have had traumatic dental experiences in the past Patients who have trouble sitting still for long periods If any of these situations apply to you, sedation dentistry might be the key to finally getting the care your teeth need. Types of Sedation Used in Dentistry There isn’t just one way to achieve dental sedation. Dentists use a range of techniques depending on your level of anxiety, the complexity of the procedure, your age, and your overall health. The most common types include: 1. Nitrous Oxide (Laughing Gas) This is the most common and mildest form of sedation. It’s inhaled through a small mask placed over your nose. Nitrous oxide makes you feel light, calm, and sometimes a bit giddy. The effects wear off quickly after the mask is removed, which means you can usually drive yourself home afterward. 2. Oral Sedation (Pill Form) Oral sedation involves taking a prescription pill, usually about an hour before your appointment. A common medication used is Halcion, which is in the same drug family as Valium. It makes you drowsy, and in higher doses, some people fall asleep during the procedure. You’ll need someone to drive you to and from the appointment. 3. IV Sedation With IV sedation, the sedative is administered directly into your bloodstream. This method works quickly and gives the dentist better control over your level of sedation. You’ll remain conscious, but you may not remember the procedure. This option is usually used for longer or more complex treatments. 4. General Anesthesia This is the deepest level of sedation and is used in rare cases, often in a hospital setting. You’ll be completely unconscious during the procedure. It’s generally reserved for patients with special needs, extreme dental fear, or complex surgical cases. What Happens Before Sedation Dentistry? Before your procedure, your dentist will take a full medical history and ask about any medications you’re taking. This is to make sure the sedation option is safe for you. You’ll also talk about your level of fear or anxiety so the dentist can recommend the best type of sedation. If you’re going to be sedated through oral medication or IV, you’ll likely be asked not to eat or drink anything for several hours before the appointment. You’ll also need to arrange a ride home, since you won’t be able to drive yourself. What to Expect During the Procedure When your procedure starts, the sedation will already be in effect. Depending on the type used, you may feel sleepy, relaxed, or slightly unaware of your surroundings. Some people don’t even remember having the work done. Even under sedation, your dentist and dental team will keep a close watch on your heart rate, breathing, and blood pressure. Your safety and comfort are top priorities throughout the entire process. You’ll still receive local anesthesia (a numbing shot) to block pain during the dental work. The sedation helps with your anxiety and comfort, while the anesthesia prevents any discomfort in your mouth. Recovery After Sedation Recovery time depends on the type of sedation used. With nitrous oxide, you’ll feel normal almost immediately after the mask is removed. For oral and IV sedation, it may take a few hours before you feel completely awake and steady again. It’s important to take it easy for the rest of the day. You shouldn’t drive, operate machinery, or make any important decisions while the sedative is still in your system. Most people are back to normal by the next day.
Implant Screw Fracture
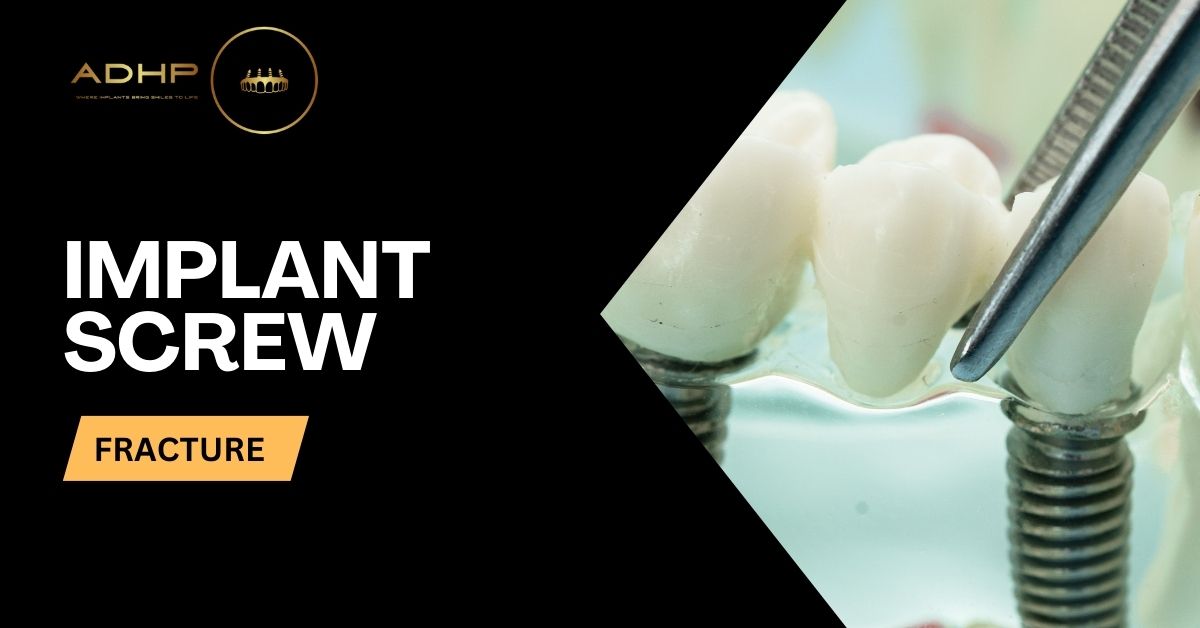
Main Takeaways: An implant screw fracture occurs when the small screw connecting implant parts cracks or breaks, compromising stability. Causes include excessive bite force, poor implant placement, ill-fitting crowns, weak bone support, and material defects. Symptoms may include loosening crowns, clicking sounds, discomfort, swelling, or tooth movement. Diagnosis often involves X-rays, CBCT scans, and clinical exams, sometimes discovering fractures during crown removal. Treatment options range from screw replacement to full implant removal, depending on severity and accessibility. Prevention includes night guards for teeth grinding, regular checkups, avoiding hard objects, and choosing skilled specialists. Early intervention is key—delaying treatment can worsen damage and complicate repair. Dental implants have become one of the most reliable ways to replace missing teeth. They are durable, natural-looking, and help restore function and confidence. However, like any medical procedure, implants can have complications. One of the more serious but less common problems is an implant screw fracture. This blog post will explain what an implant screw fracture is, why it happens, how to spot the signs early, and what treatment options are available. Whether you already have an implant or are thinking about getting one, understanding this issue can help you make informed decisions about your oral health. What Is an Implant Screw Fracture? A dental implant is made up of three main parts: the implant (which is inserted into the jawbone), the abutment (which connects the implant to the crown), and the crown (the part that looks like a tooth). The screw plays a critical role in holding these parts together. When that screw cracks or breaks, it’s called an implant screw fracture. This type of damage weakens the implant structure and can lead to movement, pain, or even failure of the entire implant system if not treated. Common Causes of Implant Screw Fracture Although dental implants are made with strong materials like titanium, the screws are still small and carry a lot of stress. Several things can lead to fracture over time: 1. Excessive Bite Force If you grind your teeth or bite down very hard (especially at night), the pressure can cause the screw to fatigue and eventually break. 2. Improper Placement If the implant is not placed at the right angle or depth, it can cause uneven pressure on the screw, which weakens it over time. 3. Poorly Fitted Crown or Abutment When the crown or abutment isn’t fitted correctly, the screw may be forced to support more weight than it should. 4. Inadequate Bone Support A strong implant needs a solid base. If the bone around the implant is weak or begins to shrink, it can affect how stable the screw is. 5. Material Defects or Wear Even high-quality metal can fail over time, especially if the screw has a manufacturing defect or experiences corrosion. Symptoms of a Fractured Implant Screw A screw fracture can sometimes happen without immediate pain. In other cases, it might be quite noticeable. Look out for these signs: Sudden loosening of the crown Clicking or popping sounds when chewing Pain or discomfort around the implant Inflammation or swelling in the gums Feeling that the tooth “moves” slightly Gaps developing around the implant If you notice any of these symptoms, don’t wait. A cracked or broken screw will not fix itself and usually gets worse over time. How Dentists Diagnose an Implant Screw Fracture Diagnosing a screw fracture can be tricky because the break often occurs deep inside the implant where it’s not visible. Dentists usually use a combination of the following methods: X-rays to check for gaps, misalignment, or broken parts Clinical exams to feel for movement or check bite pressure CBCT scans for a 3D view of the implant structure Sometimes, a broken screw is only discovered during an attempt to tighten or remove the implant crown. Treatment Options for a Broken Implant Screw The treatment for an implant screw fracture depends on where the break happened, how serious the damage is, and how easily the broken piece can be removed. Here are the most common solutions: 1. Screw Retrieval and Replacement If the broken piece can be removed without damaging the implant body, a new screw can be placed. This is the best-case scenario. 2. Abutment and Crown Replacement In cases where the crown or abutment is damaged too, the dentist may replace both the screw and the upper parts of the implant. 3. Removing and Replacing the Entire Implant If the fractured screw is stuck deep inside the implant and cannot be retrieved, the entire implant may need to be removed and replaced. This is more complex and may require bone grafting if bone has been lost. 4. Temporary Fixes If full removal isn’t possible right away, a dentist might temporarily stabilize the implant to reduce discomfort and prevent further damage while a long-term plan is created. Preventing Implant Screw Fractures While not every fracture can be avoided, there are ways to reduce your risk and help your implant last longer: 1. Wear a Night Guard If You Grind Your Teeth Grinding (also known as bruxism) puts tremendous pressure on dental implants. A night guard protects both natural and implanted teeth from damage. 2. Go to Regular Dental Checkups Routine visits help catch small issues before they become major problems. Your dentist will check for loose screws, unusual wear, and early signs of damage. 3. Avoid Using Your Teeth as Tools Never use your teeth (or your implants) to open packages or chew on hard items like ice or pens. 4. Choose a Skilled Implant Specialist The experience and precision of the dentist placing your implant matters. A poorly placed implant is more likely to have problems down the road. 5. Follow Aftercare Instructions Closely After your implant is placed, it’s important to follow all instructions. This includes eating soft foods for a while, avoiding certain habits, and taking medications if prescribed. Can an Implant Screw Fracture Be Fixed Without Surgery? In some cases, yes. If the screw has broken in a
Can Dental Whitening Strips Damage Teeth?
Main Takeaways: Whitening strips work by using peroxide to break down stains on tooth enamel, making teeth appear whiter. Overuse or incorrect use can lead to sensitivity, gum irritation, enamel erosion, and uneven whitening. Watch for warning signs like lingering sensitivity, gum pain, sharp toothaches, or enamel changes—stop use and see a dentist if they occur. Avoid use if you have sensitive teeth, gum disease, cavities, dental work, or are pregnant/nursing—always check with your dentist first. Safer whitening options include professional treatments, whitening toothpaste/mouthwash, and lifestyle changes to prevent stains. See your dentist first to check for dental issues and get personalized, safe whitening recommendations. Maintain your results with good oral hygiene, a stain-conscious diet, and occasional touch-ups as needed. Everyone wants a bright, sparkling smile. It makes you feel good and can boost your confidence. With so many products promising whiter teeth, whitening strips are a popular choice. They’re easy to use and seem to offer quick results right at home. But if you’re thinking about trying them, a big question might pop into your head: can whitening strips damage teeth? Let’s dig into that and figure out how to get a brighter smile safely. How Whitening Strips Work (The Basics) Before we talk about damage, it helps to know what whitening strips actually do. Most whitening strips have a thin layer of gel on them. This gel contains special ingredients, usually hydrogen peroxide or carbamide peroxide. These are the same kinds of ingredients dentists use for professional whitening, just in lower amounts. When you stick the strip to your teeth, the peroxide gel sits against your tooth enamel. Enamel is the hard, outer layer of your teeth. Over time, things like coffee, tea, red wine, and certain foods can stain this enamel, making your teeth look dull or yellow. The peroxide in the strips works like a tiny bleach. It gets into the enamel and breaks down the molecules that cause stains, making them less visible. This makes your teeth appear whiter. The strips are designed to be thin and flexible, so they fit snugly on your teeth. You usually wear them for a certain amount of time each day, as directed by the package, for a set number of days or weeks. It sounds simple, but understanding this process is key to figuring out, can whitening strips damage teeth? The Big Question: Can Whitening Strips Damage Teeth? So, back to our main question: can whitening strips damage teeth? The short answer is, it’s possible, especially if you don’t use them correctly. While most people use them without major issues, there are some risks to be aware of. The main concerns usually come from the peroxide in the strips. While it’s great at breaking down stains, it’s also a powerful chemical. Tooth Sensitivity: This is the most common side effect. You might feel a tingly or sharp pain in your teeth, especially when eating or drinking something hot or cold. This happens because the peroxide can temporarily make tiny tubes in your tooth enamel more open, exposing the sensitive inner part of your tooth. For most people, this sensitivity is temporary and goes away after they stop using the strips. But for some, it can be quite uncomfortable. Gum Irritation: Sometimes, the whitening gel can get onto your gums. Because gums are softer than teeth, the peroxide can irritate them, making them look white or inflamed. This is usually temporary, but it can be painful and might be a sign you’re not applying the strips correctly or that they’re too strong for your gums. Enamel Erosion (Rare but Serious): This is a more serious concern, though it’s less common with proper use. If you use whitening strips too often, for too long, or if the product is too strong, there’s a small risk that the peroxide could start to wear away your tooth enamel. Enamel does not grow back. Once it’s gone, it’s gone. Thinning enamel can lead to permanent sensitivity, make your teeth look more yellow (because the darker layer underneath shows through), and increase your risk of cavities. Uneven Whitening: Strips are flat, and teeth aren’t. They might not cover every curve or gap on your teeth perfectly. This can lead to a splotchy or uneven white appearance. Also, if you have dental work like fillings, crowns, or veneers, whitening strips won’t change their color. This means your natural teeth might get whiter, but your dental work will stay the same shade, leading to a noticeable mismatch. So, while whitening strips are generally considered safe for most people when used as directed, ignoring the instructions or overdoing it definitely increases the chance of problems. This is why knowing the answer to can whitening strips damage teeth is so important before you start. Signs of Trouble: When Whitening Strips Might Be Harming Your Teeth It’s helpful to know what signs to watch for if you’re worried about can whitening strips damage teeth. If you notice any of these, it’s a good idea to stop using the strips and talk to your dentist. Increased or Lingering Sensitivity: If your teeth become very sensitive to hot or cold, or if the sensitivity doesn’t go away after a day or two of not using the strips, that’s a warning sign. Gum Pain or Whitening: If your gums start to hurt, look irritated, or turn white where the strip has touched them, it means the peroxide is irritating your gum tissue. Sharp, Shooting Pains: While some dull sensitivity is common, sharp, sudden pains (especially when breathing in cold air or drinking) could signal more irritation to the tooth nerve. Changes in Enamel Texture: If your teeth feel rough, chalky, or look dull even after rinsing, it might be a sign of enamel changes. Dark Spots or Translucency: In very rare cases, if enamel is severely eroded, teeth might look more transparent at the edges, or underlying darker dentin might show through in spots. Existing Dental Issues Getting Worse: If you
Getting a Cavity Filled: Composite Filling

Main Takeaways Composite fillings are tooth-colored and made from a blend of plastic and glass, offering a natural look and strong bond to your tooth. They are a popular alternative to amalgam (silver) fillings because they preserve more of the natural tooth, bond directly, and contain no metal or mercury. The procedure involves removing decay, applying the composite in layers, and hardening it with a special light for a durable finish. With proper care, composite fillings typically last 5–10 years, depending on factors like location, oral hygiene, and chewing habits. Benefits include aesthetic appeal, conservative treatment, versatility, and less sensitivity to temperature changes compared to metal fillings. Drawbacks may include higher cost, longer placement time, potential staining, and slightly less durability in large, high-pressure fillings. Regular dental checkups, good oral hygiene, and avoiding hard foods help extend the life of your composite filling. ADHP – Torrance offers expert dental care and personalized guidance on choosing the right filling for your smile and needs. Nobody likes getting a cavity. That little hole in your tooth can be annoying, sometimes painful, and definitely something you want to fix. When you visit the dentist to get a cavity repaired, one of the most common solutions they offer is a composite filling. These tooth-colored fillings are popular for many reasons, but what exactly are they, and what should you know about them? Let’s talk about how these fillings work to fix your teeth and keep your smile looking great. What Exactly is a Composite Filling? When a dentist talks about a composite filling, they’re talking about a special kind of tooth repair that blends right in with your natural teeth. Unlike the old silver fillings (called amalgam fillings), composite fillings are made from a mix of plastic and fine glass particles. This mix can be colored to match the exact shade of your tooth, making it almost invisible when you smile. Think of it like this: when you have a cavity, it’s a hole caused by decay. The dentist first cleans out all the decayed (bad) part of your tooth. Then, they fill that space with the composite material. This material is soft at first, like a thick paste. The dentist shapes it to fit perfectly into the hole and match the natural curves of your tooth. Once it’s in place, they shine a special blue light on it. This light makes the composite material harden very quickly, becoming strong and durable. Because of its color-matching ability and the way it bonds to your tooth, a composite filling is a popular choice for fixing cavities, especially on your front teeth where they show, or even on back teeth where you want a natural look. Why Dentists Use Composite Fillings: The Big Benefits The reason so many dentists and patients choose a composite filling comes down to several important advantages. These fillings offer more than just fixing a hole; they help keep your smile looking its best. They Blend In: This is probably the biggest reason people love composite fillings. Since they can be matched to the exact color of your natural teeth, a composite filling is nearly invisible. You can laugh, talk, and smile wide without worrying about dark spots showing in your mouth. This is a huge plus, especially for cavities on front teeth or any part of your smile that people see. They Save More Tooth: With old silver fillings, dentists sometimes had to remove more healthy tooth material just to make sure the filling would stay in place. A composite filling actually bonds directly to the tooth structure. This means the dentist only needs to remove the decayed part of the tooth, leaving more of your healthy tooth untouched. Keeping more of your natural tooth is always better for the tooth’s long-term strength. They Bond to Your Tooth: The way composite material sticks directly to the tooth makes the tooth stronger. It helps support the remaining tooth structure and protects it from breaking. This bond also seals the tooth better, helping to keep out bacteria that could cause new decay under the filling. No Metal, No Mercury: Some people worry about the mercury content in old silver (amalgam) fillings. While dental organizations say amalgam fillings are safe, many people prefer a metal-free option. A composite filling offers this, as it contains no metal. This also means you don’t have to worry about the filling expanding and contracting as much with temperature changes, which could sometimes lead to cracks in your tooth with old metal fillings. Versatile Use: Besides filling cavities, composite material can also be used for other dental fixes. Dentists can use it to repair chipped or broken teeth, to fill in small gaps between teeth, or even to change the shape of teeth. This makes a composite filling a very flexible tool for improving smiles. These benefits make a composite filling a top choice for modern dental care, helping you keep both your oral health and your smile looking good. The Process: Getting a Composite Filling Getting a composite filling is a common and straightforward procedure that most people go through without much fuss. Here’s a step-by-step look at what happens during your dental visit: Numbing the Area: First, your dentist will usually numb the area around the tooth that needs work. They’ll use a local anesthetic, which is a special medicine that makes your tooth and gums feel sleepy, so you won’t feel any pain during the procedure. You might feel a small pinch when the shot goes in, but then the area will quickly go numb. Removing Decay: Once the area is numb, the dentist will carefully use a drill or other tools to remove all the decayed or damaged part of your tooth. They need to make sure every bit of the cavity is gone before they put in the new filling. Preparing the Tooth: After cleaning out the decay, the dentist will prepare the tooth surface. They might use a special gel or liquid
Bruxism Treatments: Finding Relief from Teeth Grinding and Jaw Pain

Main Takeways: Bruxism Basics: Bruxism is involuntary teeth grinding or clenching, often linked to stress, sleep disorders, or bite misalignment, and can cause tooth damage, jaw pain, and headaches. Common Symptoms: Look out for sore jaw muscles, worn or chipped teeth, tooth sensitivity, headaches, and sleep disturbances. Professional Treatments: Effective options include custom night guards, dental corrections, Botox injections, physical therapy, and treatment for underlying sleep issues. At-Home Solutions: Stress management, jaw exercises, warm compresses, avoiding stimulants, and improving sleep hygiene can help relieve symptoms. Children & Seniors: Bruxism affects all ages—kids may outgrow it, while seniors may need bite or denture adjustments due to age-related changes. Risks of Ignoring It: Untreated bruxism can lead to TMJ disorders, severe tooth wear, chronic pain, and reduced sleep quality. Why Choose ADHP – Torrance: Their expert team provides personalized, comprehensive bruxism treatment to relieve pain, restore function, and protect your long-term oral health. Do you wake up with sore jaw muscles, headaches, or worn-down teeth? You might be one of the millions of people affected by bruxism—a condition characterized by the involuntary grinding or clenching of teeth. While bruxism can affect people of all ages, it often goes undiagnosed until noticeable damage occurs. The good news? A wide range of effective bruxism treatments are available to help you find relief and protect your oral health. In this comprehensive guide, we’ll explore everything from the causes and symptoms of bruxism to the most effective professional and at-home treatment options. Whether your condition is mild or severe, there is a solution that can help you reclaim comfort, sleep better, and preserve your smile. What Is Bruxism? Bruxism is the medical term for the habitual grinding, gnashing, or clenching of teeth, typically occurring during sleep (sleep bruxism) or while awake (awake bruxism). Although occasional teeth grinding might not cause harm, chronic bruxism can lead to significant complications, including: Jaw pain and tension Tooth wear and fractures Headaches and migraines TMJ disorders Sleep disturbances Knowing what triggers bruxism is the first step toward identifying the best bruxism treatments for your specific needs. Causes of Bruxism: What’s Behind the Grinding? Bruxism can stem from a combination of physical, psychological, and genetic factors. Common causes include: 1. Stress and Anxiety One of the most frequent triggers, stress often manifests physically through jaw clenching or teeth grinding, particularly during sleep. 2. Sleep Disorders Conditions like sleep apnea, snoring, or insomnia are commonly linked with nighttime bruxism. 3. Misaligned Bite When the teeth don’t line up correctly (malocclusion), it may lead to unintentional grinding. 4. Medications and Substances Certain antidepressants, stimulants, caffeine, tobacco, and alcohol can increase the risk of bruxism. 5. Neurological Conditions In some cases, bruxism may be related to disorders such as Parkinson’s disease or ADHD. Determining the root cause is crucial for choosing effective bruxism treatments that provide lasting results. Common Symptoms of Bruxism Bruxism may develop silently over time. Recognizing the signs early can prevent permanent damage. Common symptoms include: Audible teeth grinding during sleep Flattened, chipped, or loose teeth Tooth sensitivity Tight or sore jaw muscles Clicking or popping sounds in the jaw Tension headaches Ear aches not caused by infection Sleep disturbances or daytime fatigue If any of these symptoms sound familiar, it’s time to explore bruxism treatments before more serious issues arise. Diagnosis: How Is Bruxism Identified? Dentists typically diagnose bruxism during routine dental exams. They look for telltale signs such as worn enamel, broken teeth, and jaw tenderness. In some cases, the following may be recommended: Dental X-rays to assess internal damage Sleep studies (polysomnography) to evaluate sleep bruxism and related disorders Patient questionnaires about stress levels, sleep quality, and lifestyle habitsAn accurate diagnosis ensures the most effective treatment plan is implemented. Professional Bruxism Treatments While lifestyle changes can help manage minor cases of bruxism, moderate to severe conditions often require professional intervention. Here are the most common clinical bruxism treatments: 1. Custom Night Guards A custom-fitted night guard (also called an occlusal splint) is one of the most effective ways to protect teeth during sleep. These devices cushion the teeth, preventing contact and reducing strain on the jaw muscles. Benefits: Prevents tooth damage Reduces jaw pain and muscle tension Improves sleep quality 2. Dental Corrections In cases where bruxism is caused by bite misalignment or missing teeth, dental treatments may include: Orthodontic work (braces or aligners) Crowns or reshaping of teeth Restorative procedures to rebuild damaged teeth Correcting the bite can eliminate the mechanical causes of grinding. 3. Botox Injections Botox is increasingly being used as a treatment for bruxism. When injected into the jaw muscles (masseter), Botox temporarily weakens them, reducing involuntary grinding and clenching. Benefits: Minimizes pain and headaches Protects teeth from wear Typically lasts 3-6 months per treatment 4. Physical Therapy Physical therapy for bruxism focuses on jaw relaxation techniques, muscle strengthening, and posture correction. Manual therapy and ultrasound treatments may also be used to reduce inflammation and improve jaw function. 5. Treatment for Sleep Disorders If bruxism is linked to sleep apnea or another disorder, treating the root sleep issue can resolve the grinding. CPAP machines, oral appliances, or behavioral therapy may be recommended. Holistic and At-Home Bruxism Treatments While professional care is vital for moderate to severe cases, certain lifestyle modifications and home remedies can greatly reduce bruxism symptoms or prevent its onset. 1. Stress Management Stress is one of the most common contributors to bruxism. Adopting effective stress reduction strategies can make a significant difference. Techniques include: Meditation and mindfulness Breathing exercises Yoga or tai chi Journaling Talking with a therapist Reducing stress helps calm the central nervous system and reduces unconscious clenching. 2. Jaw Exercises and Relaxation Stretching and relaxing the jaw muscles can ease tension and improve range of motion. Try this daily routine: Gently massage your jaw and temples Open your mouth wide and hold for a few seconds Move your jaw from side to side slowly Practice gentle breathing while resting your tongue on the roof of your mouth
Tartar Removal: A Healthy Smile Starts Here

Main Takeaways: Tartar is hardened plaque that forms quickly and can only be removed by a dental professional—not by brushing or flossing. Tartar buildup can lead to serious oral and systemic health issues, including gum disease, tooth decay, bad breath, and increased risk of heart disease and diabetes. Professional cleanings, including scaling and root planing, are essential for removing tartar and maintaining gum health. Prevention starts at home with daily brushing, flossing, a balanced diet, and avoiding sugary, sticky foods. Lifestyle habits like smoking accelerate tartar formation and interfere with healing—quitting greatly improves oral health. Children and dental implants are also vulnerable to tartar buildup, so consistent care is necessary across all age groups and dental conditions. Regular dental visits (every 6 months or as needed) and choosing an experienced provider like ADHP – Fallbrook are key to long-term oral health. Maintaining a radiant, healthy smile goes beyond just brushing and flossing. One of the most overlooked yet essential components of oral hygiene is tartar removal. Tartar, also known as dental calculus, is a hardened form of plaque that adheres stubbornly to teeth and can lead to serious dental issues if left untreated. Understanding how tartar forms, the dangers it poses, and how to remove and prevent it is crucial for anyone aiming to preserve their oral health long-term. Explore everything you need to know about tartar removal. From professional treatments and at-home prevention to the long-term effects of ignoring buildup. Let’s dive in and uncover the secrets to maintaining a cleaner, healthier smile. What Is Tartar and How Does It Form? Tartar is the calcified version of plaque—a sticky film composed of bacteria, food particles, and saliva. When plaque isn’t removed through proper brushing and flossing, it hardens within 24 to 72 hours and becomes tartar. Once formed, tartar cannot be removed by brushing alone and requires professional dental tools for complete removal. It typically accumulates along the gumline, between teeth, and in hard-to-reach areas of the mouth. The rough surface of tartar makes it easier for more plaque to accumulate, creating a vicious cycle that increases your risk for tooth decay, gum disease, and even systemic health problems. Why Tartar Removal Is So Important Tartar doesn’t just affect the appearance of your teeth—it poses serious threats to your oral and overall health. Here are some key reasons why tartar removal is crucial: Prevents Gum Disease: Tartar buildup irritates and inflames the gums, potentially leading to gingivitis or the more severe periodontitis. Reduces Bad Breath: Bacteria trapped in tartar can emit foul-smelling compounds. Protects Tooth Enamel: Tartar harbors acids that can erode enamel and lead to cavities. Improves Aesthetics: Tartar can appear yellow or brown, affecting the appearance of your smile. Minimizes Risk of Systemic Conditions: Poor oral health has been linked to heart disease, diabetes, and respiratory infections. By making tartar removal a priority, you protect more than just your teeth—you’re investing in your total body health. Professional Tartar Removal: What to Expect at the Dentist Once tartar has formed, only a dental professional can remove it effectively. During a dental cleaning, your hygienist uses specialized instruments to gently scrape away tartar from above and below the gumline. Scaling and Root Planing For more extensive buildup, especially beneath the gums, a deeper cleaning procedure known as scaling and root planing may be recommended. This involves: Scaling: Removing tartar from the surface of teeth and under the gumline. Root Planing: Smoothing the tooth roots to prevent future plaque adhesion. This method not only removes existing tartar but also helps reduce inflammation and allows the gums to reattach to the teeth. Can You Remove Tartar at Home? While brushing and flossing can prevent tartar from forming, they cannot eliminate it once it has hardened. However, certain products and habits can help slow down or minimize buildup. Dental Tools for At-Home Maintenance Some over-the-counter dental kits include scraping tools or tartar-control toothpastes. These can be helpful when used correctly, but improper use can damage enamel or gums. Always consult your dentist before attempting at-home scraping. Natural Remedies A few natural substances are believed to help reduce plaque before it hardens: Baking soda: Neutralizes acids and provides mild abrasion. Hydrogen peroxide: Helps reduce bacteria when diluted and used as a rinse. Oil pulling: Swishing coconut or sesame oil may reduce oral bacteria, though it doesn’t remove tartar. These methods can support your dental care routine, but they are not substitutes for professional tartar removal. The Role of Diet in Tartar Prevention What you eat plays a significant role in your oral health. Some foods encourage plaque formation, while others can help fight it. Foods That Promote Tartar Buildup Sugary snacks and drinks Refined carbohydrates (like white bread and chips) Sticky foods that cling to teeth Foods That Help Fight Plaque Crunchy fruits and vegetables (like apples and carrots) Cheese and yogurt (rich in calcium and phosphate) Green tea (contains antioxidants that reduce inflammation and bacteria) Incorporating more tooth-friendly foods into your diet can support your body’s natural defenses against plaque and tartar. How Smoking Affects Tartar Formation Tobacco use is one of the leading risk factors for excessive tartar buildup. Smoking decreases saliva production and promotes the growth of harmful bacteria in the mouth. This combination accelerates plaque and tartar development and also interferes with healing after tartar removal procedures. Quitting smoking not only enhances the appearance of your teeth but also greatly improves your chances of maintaining long-term oral health. How Often Should You Get Tartar Removed? For most individuals, dental cleanings every six months are sufficient to manage tartar. However, some may require more frequent visits, especially if they: Smoke Have braces or retainers Suffer from chronic gum disease Experience excessive plaque buildup Your dentist will recommend the ideal frequency based on your oral health status. Regular appointments ensure tartar is addressed before it leads to serious complications. Tartar vs. Plaque: What’s the Difference? Although often used interchangeably, plaque and tartar are not the same: Plaque is a soft,
Dental Implants in Torrance, CA
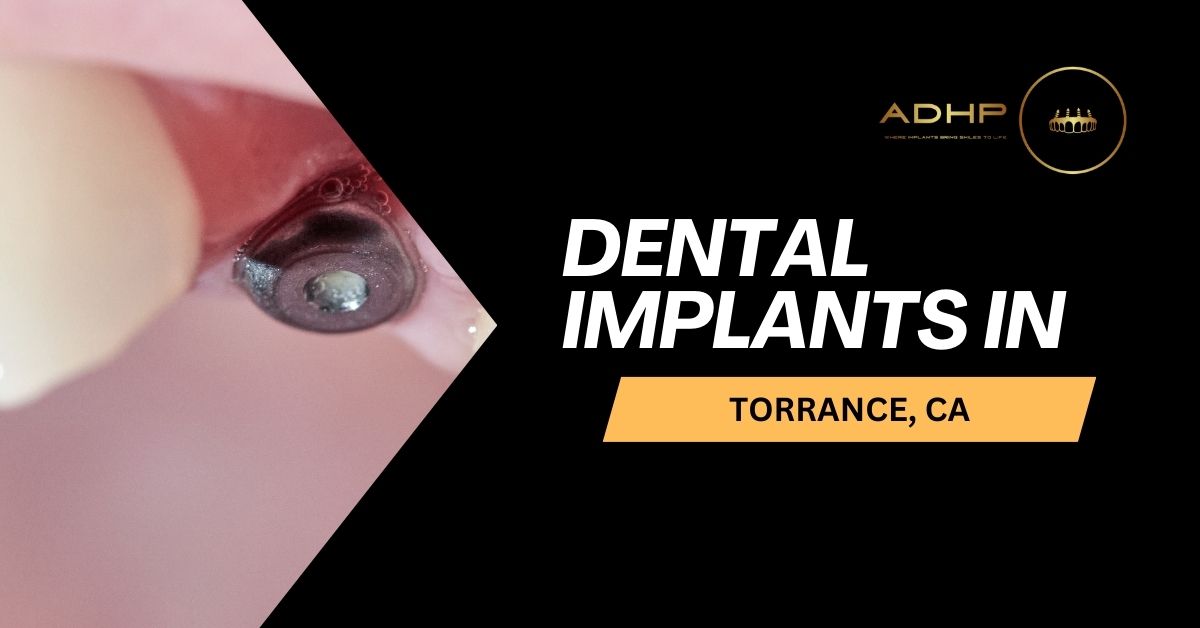
Missing teeth can have a serious impact on both your smile and your overall oral health. Whether due to injury, decay, or age, the loss of even one tooth can cause bone loss, shifting of surrounding teeth, and a drop in self-confidence. Thankfully, dental implants offer a long-lasting, natural-looking solution for replacing missing teeth. If you’re exploring dental implants Torrance CA, this comprehensive guide will help you understand the procedure, benefits, and what to expect — and why ADHP Torrance is a leading choice for implant dentistry. What Are Dental Implants? Dental implants are artificial tooth roots made from biocompatible materials like titanium. These implants are surgically placed into the jawbone where they fuse with the bone over time through a process called osseointegration. Once healed, a custom-made crown is attached to the implant, completing the restoration and delivering the look and function of a natural tooth. Unlike dentures or bridges, dental implants are designed to be permanent, offering unmatched stability and durability. Benefits of Dental Implants Dental implants are widely considered the gold standard for tooth replacement, and for good reason. Here are some of the top benefits: 1. Natural Appearance and Function Implants look, feel, and function like your natural teeth. You can eat, speak, and smile with confidence without worrying about slipping or clicking. 2. Bone Preservation When a tooth is lost, the jawbone underneath begins to deteriorate. Dental implants stimulate the bone just like natural teeth, helping to preserve bone density and facial structure. 3. Long-Term Solution With proper care, dental implants can last 20 years or longer. They offer a better return on investment over time compared to other restorations that may need to be replaced more frequently. 4. Improved Oral Health Unlike bridges that require altering adjacent teeth, implants stand alone. This helps preserve the integrity of your natural teeth and simplifies oral hygiene routines. Are You a Candidate for Dental Implants? If you’re considering dental implants Torrance CA, the first step is to determine whether you’re a good candidate for the procedure. Ideal candidates typically have: One or more missing teeth Healthy gums free from periodontal disease Adequate jawbone density to support the implant Good overall health and no uncontrolled chronic conditions Even if you’ve been told in the past that implants aren’t an option, advances in bone grafting and implant technology may change that. It’s worth consulting a specialist to explore your options. The Dental Implant Process: What to Expect Getting dental implants is a multi-step process that takes place over several months. Here’s a general overview of what to expect: 1. Consultation and Imaging During your initial visit, the implant specialist will perform a thorough examination, take X-rays or 3D scans, and develop a customized treatment plan. 2. Implant Placement The implant is surgically inserted into the jawbone under local anesthesia or sedation. After placement, the healing process can take 3 to 6 months as the implant integrates with the bone. 3. Abutment Placement Once the implant is securely fused, a small connector piece called an abutment is attached to it. This will hold the final crown in place. 4. Crown Placement Finally, a custom-made dental crown is attached to the abutment, completing your new smile. Dental Implants vs. Other Tooth Replacement Options To fully appreciate the value of dental implants Torrance CA, it helps to compare them with other common alternatives: Dentures Less expensive upfront Prone to slipping and discomfort Require adhesives May cause bone loss over time Dental Bridges Fixed in place and more stable than dentures Requires altering healthy adjacent teeth May not last as long as implants Does not prevent bone loss in the missing tooth area Implants Most natural and permanent solution Preserve bone and adjacent teeth Higher upfront cost but better long-term value When you factor in comfort, function, aesthetics, and long-term health benefits, implants are often the most effective solution. Cost of Dental Implants in Torrance, CA The cost of dental implants Torrance CA can vary depending on several factors, including: Number of implants needed Complexity of the case Need for bone grafting or sinus lifts Type of restoration (single crown, bridge, full arch) Dentist’s expertise and location On average, a single dental implant in the U.S. can range from $3,000 to $5,000. While the initial cost may seem high, implants tend to save money over time by reducing the need for replacements and additional dental work. Some insurance plans may cover a portion of the procedure, especially if it’s deemed medically necessary. Many Torrance dental offices also offer financing options or payment plans to make the procedure more accessible. How to Choose the Right Implant Dentist in Torrance Not all dental professionals are equally qualified to perform implant surgery. When choosing a provider for dental implants Torrance CA, consider the following: Experience and Credentials Look for a dentist who specializes in implant dentistry and has extensive training, preferably from organizations like the American Academy of Implant Dentistry (AAID) or the International Congress of Oral Implantologists (ICOI). Technology and Equipment Advanced diagnostic tools like 3D imaging and digital planning systems lead to more precise and successful outcomes. Patient Reviews Check online reviews and testimonials to gauge patient satisfaction and overall experience. Customized Care Choose a practice that takes the time to explain your options, listens to your concerns, and provides a tailored treatment plan that aligns with your goals. Post-Implant Care and Maintenance After receiving dental implants, proper care is crucial to ensure long-term success. Fortunately, maintenance is quite similar to caring for natural teeth: Brush twice daily with a soft-bristled toothbrush Floss daily or use an interdental brush Visit your dentist regularly for cleanings and check-ups Avoid smoking, which can interfere with healing Protect your implants from grinding or clenching (a nightguard may be recommended) With good oral hygiene and regular dental visits, your implants can serve you well for decades. Why Choose ADHP for Dental Implants in Torrance, CA? If you’re searching for dental implants Torrance CA, ADHP Torrance offers
Can Wisdom Teeth Cause Gum Recession? Understanding the Connection

Wisdom teeth, also known as third molars, often spark a number of oral health concerns as they begin to emerge in late adolescence or early adulthood. From overcrowding to infection, the complications surrounding these molars are well-documented. However, one question many patients ask their dentists is: can wisdom teeth cause gum recession? The short answer is yes, but the issue is more complex and involves various factors that intertwine oral hygiene, jaw structure, and the position of the teeth themselves. Let’s look into the connection between wisdom teeth and gum recession, identify the warning signs, and discuss available treatment options. We’ll also cover preventative measures to help you maintain a healthy smile—and why consulting with a dental expert like ADHP – Fallbrook can make all the difference. What Is Gum Recession? Before we dive into the connection, it’s essential to understand what gum recession is. Gum recession occurs when the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or its root. This can lead to increased sensitivity, higher risk of decay, and even tooth loss if left untreated. Gum recession isn’t always immediately noticeable. Some of the early signs include: Increased tooth sensitivity Visibly longer teeth Discomfort near the gumline Swollen or inflamed gums Bleeding after brushing or flossing The causes of gum recession can range from poor oral hygiene to aggressive brushing, periodontal disease, tobacco use, and genetic predisposition. But one commonly overlooked cause is the impact of wisdom teeth. How Can Wisdom Teeth Cause Gum Recession? So, can wisdom teeth cause gum recession? Absolutely. Wisdom teeth can contribute to gum recession in several ways, especially when they are impacted, partially erupted, or growing at awkward angles. 1. Impacted Wisdom Teeth and Pressure on Adjacent Teeth Impacted wisdom teeth don’t fully break through the gum line, often because they don’t have enough room to emerge. This condition can create pressure on the surrounding molars. As the pressure builds, it can disrupt the alignment of your teeth and cause the gums to recede, especially around the second molars. 2. Increased Inflammation and Infection Risk When wisdom teeth are partially erupted, they create a flap of gum tissue that traps food and bacteria. This area is incredibly difficult to clean and becomes a breeding ground for infection. The resulting inflammation can damage the surrounding gum tissue and lead to recession if not treated promptly. 3. Misalignment and Gum Trauma Wisdom teeth that grow at an angle may push against neighboring teeth. This pressure doesn’t just affect tooth alignment—it also strains the gum tissue, making it more likely to recede due to constant friction or trauma. 4. Periodontal Pockets Near Wisdom Teeth The space around erupting wisdom teeth can form what’s known as a periodontal pocket—a gap that allows bacteria to accumulate and degrade the supporting gum tissue and bone. If this pocket isn’t cleaned or treated, it can evolve into a serious infection and contribute to receding gums. Signs That Wisdom Teeth May Be Affecting Your Gums Identifying potential problems early is critical to preserving your oral health. Here are some signs that your wisdom teeth may be contributing to gum recession: Persistent bad breath or bad taste in the mouth Swelling in the back of the mouth or jaw Pain or discomfort when chewing Bleeding or tender gums near the wisdom teeth Difficulty opening your mouth fully Noticeable gum recession around nearby teeth If you’re experiencing any of these symptoms, it’s best to schedule a consultation with a dental professional. They can evaluate whether your wisdom teeth are the root cause of your gum issues. Preventative Measures to Avoid Gum Recession from Wisdom Teeth The best way to address gum recession caused by wisdom teeth is to prevent it before it starts. Here are a few proactive steps to consider: Regular Dental Check-Ups Routine dental exams allow your dentist to monitor the growth and positioning of your wisdom teeth through X-rays. Early detection of alignment issues or impaction can help prevent gum recession before it begins. Improved Oral Hygiene Keeping the back of your mouth clean is crucial. Because wisdom teeth are difficult to reach, they are more susceptible to plaque buildup. Use a soft-bristled toothbrush, floss daily, and consider a water flosser to remove debris around those hard-to-reach areas. Timely Removal of Wisdom Teeth In many cases, dentists recommend removing wisdom teeth before they can cause problems. If there’s a high risk that they’ll damage adjacent teeth or contribute to gum recession, preemptive extraction may be the best course of action. Avoiding Tobacco Products Smoking and chewing tobacco weaken the gums and make it harder for the mouth to fight off infection. Quitting these habits can significantly reduce your risk of both gum disease and gum recession. Treatment Options for Gum Recession If gum recession has already occurred—whether due to wisdom teeth or other causes—it’s important to explore treatment options. Depending on the severity, your dentist may recommend one or more of the following: Scaling and Root Planing This deep-cleaning technique removes plaque and tartar from below the gum line, helping to reduce inflammation and promote healing in mild to moderate cases of recession. Gum Graft Surgery For more severe cases, a gum graft may be necessary. This procedure involves taking tissue from another part of the mouth and attaching it to the affected area to cover exposed roots and strengthen the gum line. Antibiotic Therapy If infection is present, your dentist may prescribe antibiotics to kill the bacteria and reduce inflammation. This is often used alongside other treatments. Wisdom Tooth Extraction If wisdom teeth are found to be the root cause of gum issues, their removal can prevent further damage and support gum tissue recovery. Post-extraction care is essential to ensure proper healing and prevent additional complications. Why Prompt Action Is Important Waiting too long to address gum recession can result in irreversible damage. Not only can this lead to increased sensitivity and discomfort, but it also raises your risk

