Tooth Pain When Chewing: 7 Possible Causes (And What to Do Next)

Introduction Tooth pain when chewing is one of the most common—and most frustrating—dental issues. It might feel like a sharp jolt, a dull ache, or pressure that only shows up when you bite down. The problem is that this type of pain is rarely random. In most cases, it’s your body signaling that something deeper needs attention. In this guide, we’ll break down the 7 most common causes of tooth pain when chewing, how to identify them, and when it’s time to see a dentist. What Does Tooth Pain When Chewing Mean? Pain while chewing typically indicates: Damage to the tooth structure Inflammation or infection Issues with surrounding gums or bone The key detail is that pain under pressure usually points to a structural issue rather than simple sensitivity. 7 Possible Causes of Tooth Pain When Chewing 1. Tooth Decay (Cavities) Cavities are one of the most common causes of tooth pain, especially when pressure is applied during chewing. As decay progresses, it weakens the outer enamel and exposes more sensitive inner layers of the tooth. Cavities weaken the enamel and expose the inner layers of the tooth. When you chew, pressure hits these sensitive areas. Learn more: https://www.nidcr.nih.gov/health-info/tooth-decay Signs: Sharp or localized pain Sensitivity to sweets or temperature Visible holes or discoloration Treatment: Fillings (early stage) Crowns (advanced cases) 2. Cracked Tooth A cracked tooth can be difficult to detect but is a frequent cause of pain when chewing. The crack may not be visible, yet it can allow pressure to affect the inner structures of the tooth. A cracked tooth can cause pain only when biting—especially when releasing pressure. Learn more: https://my.clevelandclinic.org/health/diseases/10997-cracked-tooth Signs: Pain when chewing, but not constant Sensitivity to hot/cold No obvious visible damage Treatment: Dental crown Root canal (if nerve affected) 3. Loose or Damaged Filling Fillings are not permanent and can wear down or break over time. When this happens, the underlying tooth may become exposed and sensitive to pressure. Old fillings can crack or loosen over time, exposing sensitive areas. Learn more: https://www.mouthhealthy.org/en/az-topics/f/fillings Signs: Pain when biting Food getting stuck Rough or uneven tooth surface Treatment: Replace filling Upgrade to crown if needed 4. Gum Disease (Periodontal Issues) Gum disease affects the tissues and bone that support your teeth. As it progresses, it can cause instability, making chewing uncomfortable or painful. When gums and supporting bone weaken, teeth become unstable—making chewing painful. Learn more: https://www.cdc.gov/oralhealth/conditions/periodontal-disease.html Signs: Swollen or bleeding gums Bad breath Loose teeth Treatment: Deep cleaning (scaling & root planing) Ongoing periodontal care 5. Tooth Abscess (Infection) An abscess is a serious dental infection that develops at the root of a tooth or between the gum and tooth. This condition can cause intense pain, especially when chewing. An abscess is a serious infection at the root of the tooth. Learn more: https://www.mayoclinic.org/diseases-conditions/tooth-abscess Signs: Severe pain when chewing Swelling in gums or face Fever or bad taste This is urgent and should not be delayed. Treatment: Root canal Antibiotics Extraction (if necessary) 6. Bite Misalignment (Occlusion Issues) When your bite is not properly aligned, certain teeth can absorb more force than they should. Over time, this uneven pressure can lead to pain when chewing. If your bite is off, certain teeth absorb too much pressure. Learn more: https://www.ncbi.nlm.nih.gov/books/NBK557634/ Signs: Pain in one specific tooth Jaw discomfort Uneven wear on teeth Treatment: Bite adjustment Night guard (if grinding involved) 7. Tooth Sensitivity or Worn Enamel Enamel naturally wears down over time or due to habits like grinding or acidic foods. When this protective layer is reduced, the tooth becomes more sensitive to pressure and temperature. Enamel loss exposes dentin, making pressure and temperature more painful. Learn more: https://www.nidcr.nih.gov/health-info/tooth-sensitivity Signs: Mild to moderate discomfort Triggered by hot, cold, or pressure No visible damage Treatment: Desensitizing toothpaste Fluoride treatments Bonding or crowns in severe cases When Should You See a Dentist? You should schedule an appointment if: Pain lasts more than 1–2 days It’s getting worse There’s swelling or fever You avoid chewing on one side Pain is your body’s warning system and should not be ignored. How Dentists Diagnose the Problem Your dentist may use: X-rays Bite tests Visual examination Sensitivity testing The goal is to identify the exact source rather than simply treating symptoms. Treatment Options (Depending on Cause) Treatment may include: Fillings or crowns Root canal therapy Gum treatment Bite adjustment Tooth replacement (in severe cases) How to Prevent Tooth Pain When Chewing Brush twice daily Floss regularly Avoid chewing hard objects (ice, pens) Visit your dentist every 6 months Address small issues early Prevention is always more effective and less costly than treatment. Conclusion Tooth pain when chewing is never something to ignore. Whether it’s a minor cavity or a more serious issue like a cracked tooth or infection, early treatment makes all the difference. If you’re experiencing discomfort when biting or chewing, schedule an evaluation at one of our convenient locations: Fallbrook Office: https://www.adhp.com/fallbrook-dentist/ Torrance Office: https://www.adhp.com/dentist-in-torrance-ca/ Early diagnosis can prevent more serious issues and help restore your comfort quickly.
Loose Tooth in Adults: What to Do and When to See a Dentist

Introduction A loose tooth as an adult can feel alarming—and for good reason. Unlike children, adult teeth are meant to be permanent. If one starts to feel loose, it’s usually a sign that something isn’t right beneath the surface. The good news is that not all loose teeth need to be removed. In many cases, early action can stabilize the tooth and prevent further damage. In this guide, we’ll explain the most common causes of a loose tooth, what you should do right away, and when it’s time to see a dentist. Is a Loose Tooth Always Serious? A loose tooth in adults is almost always a warning sign, but that doesn’t mean the tooth is beyond saving. The severity depends on the cause and how quickly the issue is addressed. In some cases, looseness is temporary and treatable. In others, it may indicate more advanced conditions such as infection or bone loss. The key is identifying the cause early and taking the right steps to protect the tooth. Common Causes of a Loose Tooth in Adults There are several reasons why a tooth may become loose. Understanding the underlying cause is essential for determining the right treatment. 1. Gum Disease (Periodontal Disease) Gum disease is the leading cause of loose teeth in adults. As the infection progresses, it damages the gums and the bone that supports your teeth. As support weakens, teeth can begin to shift or feel loose. Learn more: https://www.cdc.gov/oralhealth/conditions/periodontal-disease.html Signs: Bleeding or swollen gums Receding gums Persistent bad breath Teeth shifting or loosening Treatment: Deep cleaning (scaling and root planing) Ongoing periodontal care Advanced treatment in severe cases 2. Trauma or Injury A blow to the mouth or excessive force can damage the structures that hold a tooth in place. Even if the tooth looks intact, the supporting ligaments may be affected. 3. Teeth Grinding (Bruxism) Chronic grinding or clenching puts excessive pressure on your teeth and supporting structures. Over time, this can weaken the attachment and lead to looseness. This often happens during sleep, making it difficult to detect early. Learn more: https://www.nidcr.nih.gov/health-info/bruxism Signs: Jaw pain or tightness Worn or flattened teeth Headaches Tooth sensitivity Treatment: Night guard Bite adjustment Stress management 4. Infection or Abscess A dental infection can weaken the bone and tissue surrounding a tooth, causing it to become loose. This is a serious condition that requires prompt treatment. Learn more: https://www.mayoclinic.org/diseases-conditions/tooth-abscess Signs: Pain or pressure Swelling in gums or face Fever or bad taste Treatment: Root canal Antibiotics Extraction (if necessary) 5. Bone Loss in the Jaw Bone loss can occur due to untreated gum disease or long-term missing teeth. When there isn’t enough bone to support the tooth, it may begin to loosen. This process is often gradual but can become severe over time. Learn more: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6874992/ Signs: Changes in bite Gum recession Tooth movement Treatment: Bone grafting Periodontal treatment Tooth replacement options What to Do If You Have a Loose Tooth If you notice a loose tooth, taking the right steps immediately can make a big difference in the outcome. Do: Avoid chewing on the affected side Keep the area clean with gentle brushing and flossing Eat soft foods Schedule a dental appointment as soon as possible Don’t: Wiggle or push the tooth Ignore the problem Delay treatment Even minor looseness can worsen if left untreated. Can a Loose Tooth Be Saved? In many cases, yes—a loose tooth can be stabilized if the underlying issue is treated early. Success depends on: The cause of the looseness The severity of damage How quickly treatment begins With proper care, it’s often possible to restore stability and function. When Is Tooth Removal Necessary? If the tooth cannot be saved, removal may be the best option to protect your overall oral health. This may be recommended if: Bone loss is severe Infection cannot be controlled The tooth is too damaged to repair In these cases, replacement options such as dental implants can restore both function and appearance. How to Prevent Loose Teeth Preventing a loose tooth starts with maintaining good oral health and addressing issues early. Brush and floss daily Attend regular dental checkups Treat gum disease early Wear a night guard if you grind your teeth Avoid excessive force on teeth Early prevention is the best way to avoid more complex treatment later. Conclusion A loose tooth in adults should never be ignored. While it can be a sign of a serious issue, early treatment often makes it possible to save the tooth and prevent further damage. If you’ve noticed a loose tooth or changes in how your teeth feel, scheduling an evaluation is the most important next step. You can visit one of our convenient locations: Fallbrook Office: https://www.adhp.com/fallbrook-dentist/ Torrance Office: https://www.adhp.com/dentist-in-torrance-ca/ A professional evaluation can identify the cause and help you take the right steps to protect your long-term oral health.
Dental Implants for Diabetics in Fallbrook

Main Takeaways Managing your diabetes effectively is the most critical factor in achieving successful dental implants for diabetics Patients with controlled diabetes can achieve implant success rates comparable to non-diabetic patients when working with experienced specialists The healing timeline for diabetic patients may extend longer than average, requiring patience and commitment to post-operative care Advanced imaging technology and personalized treatment planning minimize risks and optimize outcomes for diabetic implant candidates Collaboration between your dentist and physician ensures comprehensive care that addresses both your oral and overall health needs Preventive measures including meticulous oral hygiene and regular monitoring become essential for long-term implant health in diabetic patients Modern dental techniques have transformed dental implants for diabetics from a risky procedure to a predictable, life-changing treatment option Can Diabetics Get Dental Implants? Living with diabetes means making careful decisions about medical procedures, and if you’re considering tooth replacement options, you’re probably wondering whether dental implants for diabetics are safe and effective. The answer brings encouraging news. When your diabetes is well managed, dental implants can restore your smile with success rates that rival those of patients without diabetes. The connection between diabetes and dental health runs deeper than many people realize. Elevated blood glucose affects every system in your body, including your mouth. This relationship creates unique considerations for implant treatment, but it doesn’t make implants impossible. Today’s dental implant technology combined with skilled specialists who understand diabetic care makes tooth replacement achievable for most diabetic patients. Your body’s healing capacity plays a central role in implant success. Diabetes can slow this healing process and increase vulnerability to infections. However, these challenges become manageable obstacles rather than roadblocks when you maintain stable blood sugar levels and partner with an experienced dental team. The specialists at ADHP Fallbrook bring extensive experience working with diabetic patients, using proven strategies to ensure optimal outcomes. Making an informed choice about dental implants for diabetics starts with understanding how your condition affects the treatment process. This knowledge empowers you to take the necessary steps for success and sets realistic expectations about your journey toward a restored smile. The Connection Between Diabetes and Oral Health Before exploring dental implants specifically, understanding how diabetes influences your oral health helps explain why certain precautions become necessary during implant treatment. Diabetes creates a favorable environment for oral bacteria. When blood sugar levels remain elevated, your saliva contains more glucose. Bacteria thrive on this sugar, multiplying more rapidly and producing acids that attack your teeth and gums. This bacterial overgrowth increases your risk of cavities, gum infections, and other oral health problems that can complicate implant procedures. Gum disease progresses more rapidly in diabetic patients. The relationship between diabetes and periodontal disease works both ways. Diabetes makes you more susceptible to gum infections, while active gum disease makes blood sugar harder to control. This creates a challenging cycle that must be broken before implant surgery. Healthy gums provide the foundation for successful implants, making gum disease treatment a priority. Dry mouth frequently affects diabetic individuals. Many diabetes medications reduce saliva production, and high blood sugar itself can cause dry mouth. Saliva naturally cleanses your mouth and neutralizes acids, so reduced saliva flow allows bacteria to flourish. Dry mouth also makes gum tissue more fragile and prone to irritation, which can affect healing after implant placement. Nerve damage can reduce oral sensitivity. Diabetic neuropathy sometimes affects facial nerves, reducing your ability to feel pain or discomfort in your mouth. While this might sound beneficial, it actually creates risks because you might not notice early signs of infection or other problems around healing implants. Regular professional monitoring becomes even more important when sensation is compromised. According to the National Institute of Dental and Craniofacial Research, people with diabetes face increased oral health risks, making preventive care and early intervention essential components of overall diabetes management. Assessing Your Candidacy as a Diabetic Patient Not every diabetic patient faces the same level of risk when considering dental implants. Several factors determine whether you’re a good candidate and what special measures your treatment might require. Your glycemic control serves as the primary indicator. Dentists typically evaluate your recent hemoglobin A1C results to assess diabetes management. This blood test reveals your average blood sugar over approximately three months, providing a more complete picture than daily glucose readings. Most dental implant specialists prefer A1C levels under 7%, with some requesting levels below 6.5% for elective procedures. These targets indicate that your diabetes is well controlled and your body can heal effectively. The duration of your diabetes matters. People who have lived with diabetes for many years may have developed complications that affect implant success. Long-term diabetes can lead to reduced circulation, slower healing, decreased bone density, or nerve damage. Your dental team will evaluate how your diabetes has affected your overall health when creating your treatment plan. Existing complications require evaluation. If diabetes has affected your kidneys, eyes, heart, or circulation, these conditions might influence your implant treatment. For example, poor circulation in your extremities suggests blood flow problems that could affect healing in your jaw. Your dentist will work with your physician to understand your complete health picture before recommending implants. Your commitment to care determines long-term outcomes. Successful dental implants for diabetics require dedication to excellent blood sugar management, meticulous oral hygiene, and regular professional monitoring. During your consultation, your dental team will discuss these requirements honestly. If you’re ready to commit to the necessary care, you’re likely a good candidate regardless of other risk factors. Preparing Your Body for Implant Surgery Proper preparation significantly improves implant success for diabetic patients. This phase requires collaboration between you, your dentist, and your medical doctor to optimize your health before surgery. Achieving optimal glucose control takes priority. Your dentist may recommend delaying surgery if your blood sugar has been unstable. Use the preparation period to tighten your diabetes management. Monitor your glucose levels consistently, follow your prescribed diet, take medications as directed, and stay physically active. Some patients
Dental Implants for Diabetics in Torrance

Main Takeaways Dental implants for diabetics are absolutely possible with proper blood sugar management and the right dental team Well-controlled diabetes with A1C levels below 7% significantly improves implant success rates and healing outcomes Diabetics face unique challenges including slower healing, increased infection risk, and potential bone loss around implants Advanced diagnostic imaging and careful treatment planning help ensure safe, successful implant procedures for diabetic patients Working with experienced implant specialists who understand diabetes management is crucial for long-term implant success Excellent oral hygiene and regular dental visits become even more important for diabetic patients with dental implants Modern implant techniques and materials have dramatically improved outcomes for diabetic patients compared to past decades Dental Implants and Diabetes If you have diabetes and are missing teeth, you might wonder whether dental implants are a safe option for you. The good news is that dental implants for diabetics can be highly successful when your blood sugar is well controlled and you work with an experienced dental team. Understanding how diabetes affects the implant process helps you make informed decisions about restoring your smile. Diabetes affects your body’s ability to heal and fight infections. This means that any surgical procedure, including dental implant placement, requires extra care and planning. However, modern dentistry has made tremendous advances in treating diabetic patients safely and effectively. With proper management, diabetic patients can enjoy the same benefits of dental implants as non-diabetic individuals. The relationship between diabetes and oral health is complex. High blood sugar levels can damage blood vessels throughout your body, including those in your gums and jawbone. This reduced blood flow can slow healing after implant surgery and increase the risk of infection. Additionally, diabetes can contribute to bone loss in the jaw, which may affect how well implants integrate with your bone. Despite these challenges, many diabetic patients successfully receive dental implants every year. The key lies in careful planning, excellent blood sugar control, and choosing an experienced dental team. At ADHP Torrance, our specialists understand the unique needs of diabetic patients and use advanced techniques to ensure the best possible outcomes. How Diabetes Affects Dental Implant Success Understanding exactly how diabetes impacts the implant process helps you prepare properly and set realistic expectations. Several factors come into play when considering dental implants for diabetics. Blood sugar control directly affects healing. When your blood glucose levels stay elevated, your body’s natural healing processes slow down significantly. White blood cells, which fight infection and help repair tissue, don’t work as effectively in high-sugar environments. This means the bone around your dental implant takes longer to heal and bond with the titanium post, a process called osseointegration. Infection risk increases with poorly controlled diabetes. High blood sugar creates an environment where bacteria thrive more easily. Since dental implant surgery involves creating an opening in your gums and bone, the risk of bacterial infection rises. Infections can prevent proper healing and even cause implant failure if not addressed quickly. Bone density issues affect implant stability. Diabetes can contribute to reduced bone density over time, particularly in the jaw. Dental implants need sufficient bone volume and density to remain stable and functional. If diabetes has already caused significant bone loss, you might need additional procedures like bone grafting before implant placement. Gum disease occurs more frequently in diabetic patients. Research shows that diabetes and gum disease have a two-way relationship. Diabetes makes you more susceptible to gum infections, and active gum disease makes it harder to control blood sugar. Since healthy gums are essential for dental implant success, addressing any gum disease before implant surgery becomes critically important. According to the American Diabetes Association, people with diabetes are at higher risk for oral health problems, making professional dental care and good home hygiene essential. The Importance of Blood Sugar Control Your blood sugar levels before, during, and after dental implant surgery play the most significant role in determining success. This is why your dental team will work closely with your medical doctor throughout the process. Target A1C levels matter significantly. Most dental implant specialists recommend that diabetic patients have an A1C level below 7% before proceeding with implant surgery. Some dentists prefer levels below 6.5% for optimal results. The A1C test shows your average blood sugar over the past three months, giving your dental team a clear picture of how well your diabetes is controlled. Pre-surgery preparation includes close monitoring. In the weeks leading up to your implant surgery, you’ll need to check your blood sugar more frequently and maintain it within target ranges. Your dentist may ask you to provide recent blood sugar readings and possibly a current A1C test result. This information helps them decide if it’s safe to proceed or if you need more time to improve your control. Day-of-surgery management requires coordination. The stress of surgery can affect blood sugar levels, even if you’re normally well-controlled. Your dental team will discuss with your doctor whether you need to adjust your diabetes medications on surgery day. Some patients require special scheduling, such as early morning appointments, to minimize disruption to their normal eating and medication routine. Post-surgery monitoring continues throughout healing. After implant placement, maintaining stable blood sugar becomes even more important. This is when your body needs to heal the surgical site and integrate the implant with your bone. Wide blood sugar swings or persistently high levels during this critical period can compromise healing and increase complications. Preparing for Dental Implants as a Diabetic Patient Proper preparation significantly improves your chances of successful dental implants for diabetics. The preparation phase involves several important steps that require commitment and coordination between your dental and medical teams. Comprehensive health evaluation comes first. Your implant dentist will want a complete picture of your overall health, including how long you’ve had diabetes, what medications you take, and whether you have any diabetes-related complications like neuropathy or circulatory problems. Be honest and thorough when discussing your medical history, as this information directly impacts your treatment plan.
Can You Whiten Implants? Everything Torrance Patients Need to Know

Main Takeaways Dental implant crowns cannot be whitened with traditional bleaching treatments because they’re made from ceramic or porcelain materials that don’t respond to whitening agents Understanding whether you can whiten implants before getting them placed helps you plan for a bright, uniform smile from the start Professional teeth whitening should ideally happen before implant placement so your restoration can be matched to your newly whitened natural teeth Implant crowns are color-stable and resist staining better than natural teeth, maintaining their original shade for many years with proper care If your natural teeth become darker than your implant over time, whitening your surrounding teeth can restore color harmony in your smile Replacement of an implant crown is the only way to change its color if you’re unhappy with the shade after placement Working with experienced cosmetic dentists in Torrance ensures your implants blend seamlessly with your smile goals from day one Dental Implant Materials When people ask “can you whiten implants,” they’re usually wondering about the visible crown portion of the restoration. To answer this question properly, we need to understand what dental implants are made of and how these materials respond to whitening treatments. A complete dental implant system has three parts. The implant post sits in your jawbone and acts like an artificial tooth root. This titanium or ceramic post isn’t visible when you smile. The abutment connects the post to the crown and also stays hidden beneath your gum tissue. The crown is the only part you can see, and it’s what people really mean when they ask about whitening implants. Implant crowns are crafted from dental ceramics or porcelain. These materials are chosen because they look incredibly natural, resist chewing forces well, and last for many years. Dental laboratories create each crown to match the shade, shape, and translucency of your natural teeth. The result is a restoration that blends so seamlessly with your smile that most people can’t tell which tooth is the implant. Here’s the important part: these ceramic and porcelain materials don’t have the same porous structure as natural tooth enamel. Natural teeth can be whitened because bleaching agents penetrate tiny pores in the enamel and break down stain molecules. Implant crowns have a smooth, non-porous surface that whitening products simply can’t penetrate. Why Traditional Whitening Doesn’t Work on Implants The science behind tooth whitening explains why you can’t whiten implants the same way you brighten natural teeth. Professional whitening treatments and over-the-counter products rely on hydrogen peroxide or carbamide peroxide to bleach away stains. These bleaching agents work by releasing oxygen molecules that penetrate tooth enamel. Once inside, the oxygen breaks apart the chemical bonds holding stain molecules together. This process lightens the tooth’s color from within. It’s effective on natural teeth because enamel has microscopic pores that allow the whitening agent to enter. Dental ceramics and porcelain lack these pores. The material is fired at extremely high temperatures during manufacturing, creating a glass-like surface that’s completely sealed. When you apply whitening gel to an implant crown, the product just sits on the surface without penetrating. No penetration means no whitening effect. Some people worry that whitening treatments might damage their implant crowns. The good news is that professional whitening is perfectly safe for implants. It won’t harm the restoration in any way. It simply won’t change the color either. According to the American Dental Association, tooth whitening products are designed specifically for natural tooth enamel and won’t affect the color of dental restorations including crowns, veneers, or fillings. Planning Your Smile Makeover in the Right Order Understanding that you can’t whiten implants after placement changes how you should plan cosmetic dental work. The sequence of treatments matters tremendously when you want both whiter teeth and dental implants. If you’re considering dental implants and want a brighter smile, professional teeth whitening should come first. This approach allows your dentist to see exactly what shade your natural teeth reach after whitening. Then they can create your implant crown to match this brighter color perfectly. Here’s how the ideal timeline works. First, you complete your whitening treatment and wait about two weeks for the final shade to stabilize. Your teeth might appear slightly brighter immediately after whitening, but the color settles into its true final shade within a couple of weeks. During this waiting period, your dentist takes shade measurements to determine the exact color for your implant crown. Next comes implant placement if you haven’t had that done already. The implant post needs several months to integrate with your jawbone before the crown can be attached. This healing time doesn’t affect the whitening timeline since your natural teeth stay bright while you wait. Finally, your dental laboratory fabricates the crown to match your whitened teeth. When the crown is attached to your implant, it blends seamlessly with your smile. Everything matches, and you have the bright, complete smile you wanted. What If You Already Have Implants? Many Torrance patients already have dental implants and are now considering whitening. This situation is completely manageable, but it requires understanding that your implant crown will stay the same shade. If you whiten your natural teeth and they become lighter than your existing implant crown, you’ll notice a color difference. The implant will look darker or more yellow compared to your newly brightened natural teeth. This contrast becomes more noticeable if the implant is in your smile zone where people can see it easily. You have a couple of options to address this mismatch. One choice is to whiten your natural teeth only to the point where they match your existing implant. This approach keeps everything uniform, though it means your smile won’t be as bright as it could be. The other option is to whiten your natural teeth to your desired brightness and then replace the implant crown with a new one that matches the lighter shade. Your implant post and abutment stay in place. Only the crown gets replaced, which is much simpler and
Managing Patients with a Loose Implant Abutment Screw for Fallbrook Residents
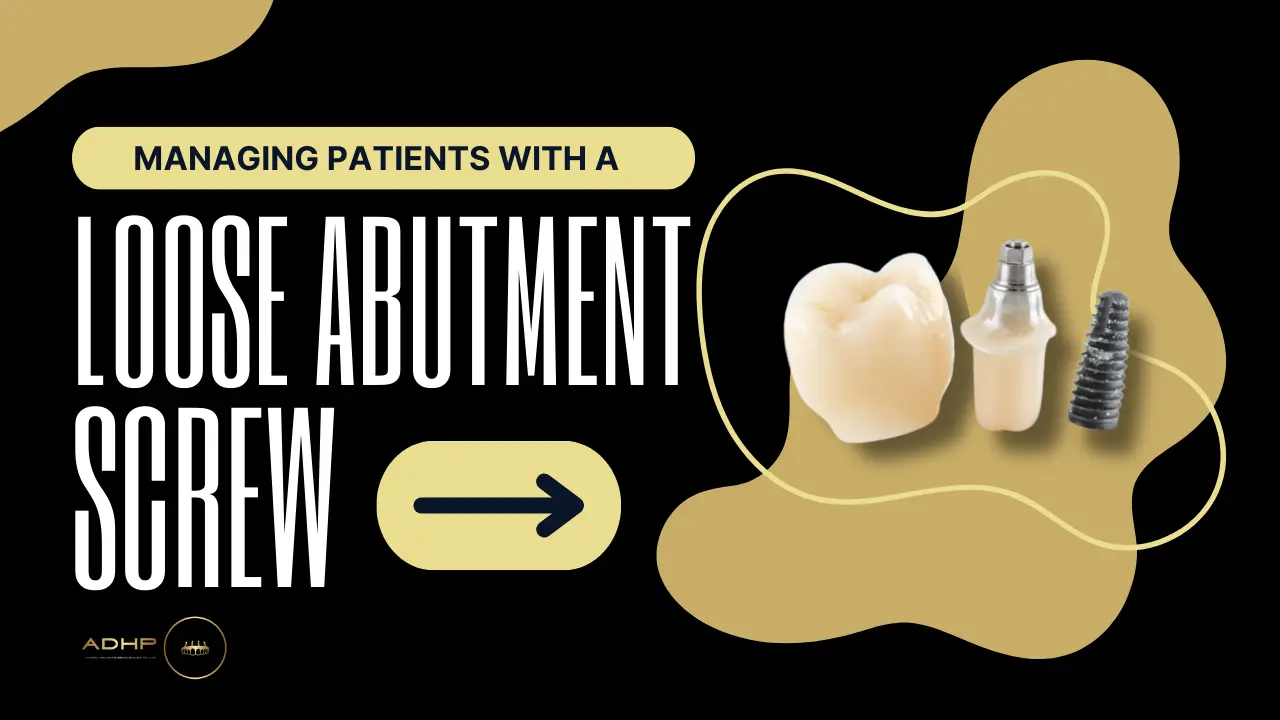
Main Takeaways A loose implant abutment screw is one of the most common mechanical complications affecting dental implants, occurring in approximately 5-12% of cases Early detection through regular dental checkups prevents more serious problems like component fracture or implant failure Patients may notice clicking sounds, movement of the crown, difficulty chewing, or discomfort when biting down on the affected implant Managing patients with a loose implant abutment screw requires prompt professional attention to prevent damage to the implant or surrounding bone Proper torque values during initial placement and regular maintenance significantly reduce the risk of screw loosening Multiple episodes of screw loosening may indicate underlying issues such as occlusal problems, component mismatch, or inadequate bone support Modern solutions include using anti-rotation devices, improved screw designs, and custom abutments that enhance stability and longevity Understanding the Implant Abutment Screw Dental implants have transformed how we replace missing teeth, giving people back their confidence and ability to eat comfortably. But like any mechanical device, implants have parts that work together, and sometimes these parts need attention. The abutment screw is a tiny but crucial component that connects the visible crown to the implant post buried in your jawbone. Think of it like a special bolt that holds everything together. The implant post acts as your new tooth root, the abutment serves as the connector piece, and the screw locks the abutment to the post. When this screw loosens, the entire restoration can become unstable. While this might sound scary, it’s actually a fairly common issue that dental professionals know how to handle effectively. In Fallbrook, where many residents choose dental implants to restore their smiles, understanding this potential complication helps patients recognize warning signs early. The good news is that managing patients with a loose implant abutment screw is straightforward when addressed quickly. Why Abutment Screws Become Loose Several factors can cause an abutment screw to loosen over time. Understanding these causes helps both patients and dental professionals prevent future occurrences. Mechanical stress from chewing creates constant forces on your dental implant. Every time you bite down, these forces transfer through the crown, down the abutment, and into the screw. Over thousands of chewing cycles, even properly tightened screws can gradually loosen. This is especially true for people who grind their teeth at night or favor one side of their mouth when eating. Improper initial torque represents another common cause. When the implant restoration is first placed, the screw must be tightened to a specific torque value measured in Newton centimeters. Too loose, and the screw will quickly loosen further. Too tight, and the screw might strip or break. Experienced implant dentists use special torque-controlled devices to ensure perfect tightening. Component mismatch can also lead to screw loosening. When the abutment doesn’t fit precisely onto the implant platform, small gaps exist that allow micro-movements. These tiny movements, repeated thousands of times during normal function, eventually loosen the screw. This is why using components from the same manufacturer and system is so important. Occlusal overload, or excessive biting forces, puts extra stress on the screw. If your bite isn’t properly balanced after implant placement, certain teeth bear more force than they should. An implant that receives too much pressure experiences accelerated screw loosening compared to implants with proper bite distribution. Recognizing the Warning Signs Patients who understand the symptoms of a loose abutment screw can seek help before the problem worsens. Early intervention makes treatment simpler and prevents additional complications. A clicking or tapping sound when you bite down often signals screw loosening. This sound happens because the crown can shift slightly on the loose abutment. Some patients describe it as feeling like their crown is “floating” or not quite attached properly. Movement of the crown represents a clear warning sign. If you can wiggle your implant crown with your tongue or finger, the abutment screw has definitely loosened. Don’t try to tighten it yourself or ignore the problem. Contact your dental provider right away. Difficulty chewing or discomfort when biting down can indicate screw loosening. The implant might feel different from your other teeth, or you might find yourself avoiding that area when eating. This protective behavior often develops subconsciously as your mouth tries to prevent further damage. Food getting trapped around the implant more than usual sometimes occurs with loose screws. As the components separate slightly, small gaps form where food particles can lodge. Increased bleeding or inflammation around the implant can follow as bacteria accumulate in these spaces. According to the American Dental Association, regular dental checkups help identify implant complications early, including screw loosening that might not yet cause obvious symptoms. The Clinical Approach to Treatment When managing patients with a loose implant abutment screw, dental professionals follow a systematic approach to diagnose and resolve the issue effectively. The initial examination includes checking the stability of the crown and taking X-rays to assess the implant and bone condition. The dentist will gently test if the crown moves and listen for sounds that indicate loosening. These diagnostic steps help determine if the problem is simply a loose screw or if other complications exist. Removing the crown comes next once loosening is confirmed. The dental team carefully unscrews and removes the crown to access the abutment screw. In some cases, the crown is cemented rather than screwed in place, which requires different removal techniques. The goal is to remove everything without damaging any components. Inspecting all components is crucial before reassembly. The dentist examines the screw, abutment, and implant platform for signs of wear, damage, or contamination. Any worn threads, cracks, or deformities mean those parts need replacement. The implant platform gets cleaned thoroughly to ensure proper contact when reassembled. Replacement of damaged parts happens when inspection reveals problems. A new screw is often recommended even if the old one looks fine, since screws can develop microscopic damage that isn’t visible to the naked eye. This small investment prevents future failures. Retightening to proper torque specifications restores stability. Using a
Family Dentist in Torrance: Comprehensive Care for Every Member of Your Family

Main Takeaways: Family dentistry provides comprehensive care for all ages, from children to seniors, eliminating the need for multiple dental offices Continuity of care allows dentists to track changes over time and detect problems early for better treatment outcomes Preventive care is the foundation of family dentistry, helping families avoid costly and invasive procedures Convenient scheduling allows multiple family members to be seen in a single visit, reducing time away from work and school Early dental visits for children build positive associations and healthy oral habits that last a lifetime Oral health is linked to overall wellness, with connections to heart disease, diabetes, and other systemic conditions Personalized care plans ensure each family member receives age-appropriate treatment and education What Is Family Dentistry Family dentistry provides dental care for patients across all age groups, eliminating the need to visit separate offices for children, teens, adults, and seniors. A family dentist is trained to manage a variety of dental needs, including preventive care, restorations, cosmetic procedures, and patient education. This approach ensures families can receive consistent dental care under one roof, making visits less stressful and more convenient. Benefits of Choosing a Family Dentist Seeing the same dental team over time offers multiple benefits: Comprehensive care: One office manages preventive, restorative, and cosmetic dental needs. Continuity of care: Dentists track changes over time and catch issues early. Convenience: Multiple family members can often be seen in a single visit. Comfort and trust: Familiarity reduces anxiety for children and adults alike. By choosing a family dentist, families can focus on prevention rather than constantly reacting to dental problems. Family Dentist in Torrance for Children Early dental care sets the foundation for a lifetime of oral health. Pediatric-focused services include gentle exams, cleanings, fluoride treatments, and sealants to prevent cavities. Family dentists in Torrance also provide guidance for parents on healthy oral habits, nutrition, and developmental concerns such as thumb sucking or pacifier use. Early education helps children build confidence and positive associations with dental visits. Preventing Cavities and Tooth Decay Children are especially prone to cavities due to developing oral hygiene skills and frequent exposure to sugary foods. A family dentist monitors risk factors and provides preventive solutions like: Fluoride treatments to strengthen enamel. Sealants to protect molars from decay. Educational guidance on brushing, flossing, and healthy eating habits. Preventive care in childhood reduces dental problems in adolescence and adulthood. Dental Care for Teens Teenagers face unique dental challenges, including orthodontic needs, sports-related injuries, and changes in oral hygiene habits. A family dentist in Torrance monitors tooth alignment, wisdom tooth development, and gum health while teaching teens responsibility for their oral care. Teen-focused guidance supports both preventive care and orthodontic success. Adult Preventive Dental Care Adults benefit from routine cleanings, examinations, and preventive treatments. Common adult dental concerns include cavities, gum disease, tooth wear, and sensitivity. Family dentistry helps adults manage these conditions with: Regular exams to detect early issues. Professional cleanings to remove plaque and tartar. Education on lifestyle factors affecting oral health, such as diet and teeth grinding. Preventive care saves time, money, and discomfort in the long run. Gum Health and Periodontal Care Gum disease can develop silently and may lead to tooth loss if untreated. A family dentist focuses on early detection and treatment of gingivitis and periodontitis. Regular cleanings, scaling, and education about proper brushing and flossing help maintain healthy gums. Strong gums support the foundation of teeth and overall oral function. Restorative Dentistry for Families When dental problems occur, restorative treatments restore function and appearance. Options may include: Fillings for cavities. Crowns to protect damaged teeth. Bonding for cosmetic improvements. Family dentists tailor treatments to age, oral health, and patient comfort, preserving natural teeth whenever possible. Dental Care for Seniors Oral health needs change with age. Seniors may face: Tooth wear and enamel thinning. Dry mouth and sensitivity. Missing teeth or the need for dentures. Family dentistry in Torrance provides solutions that address these concerns with care and respect. Maintaining oral health supports nutrition, comfort, and overall well-being. Monitoring Dental Changes Over Time Continuity of care allows a dentist to track changes in bite, tooth wear, gum health, and oral habits. Early detection of potential problems leads to simpler and more effective treatment, reducing risks of complications in the future. Education and Communication for All Ages A key part of family dentistry is educating patients. Dentists explain preventive care and procedures in age-appropriate language, helping children, teens, and adults understand their responsibilities and options. Effective communication builds trust and encourages regular visits and proper at-home oral care. Reducing Dental Anxiety Many patients experience dental anxiety, from children to adults. Family dentistry emphasizes creating a comfortable environment and familiar routines to help reduce stress. When families trust their dental provider, they are more likely to attend appointments consistently, which improves overall oral health. For patients with severe anxiety, sedation dentistry options are available to ensure comfort during dental procedures. Technology in Family Dentistry Modern family dentistry incorporates advanced technology to improve accuracy and comfort. This may include: Digital X-rays for faster, clearer imaging. Intraoral cameras to help patients see dental issues. Efficient treatment tools that minimize discomfort. Technology enhances care for patients of all ages and supports early detection and precise treatment planning. Preventive Focus in Family Dentistry Prevention is the foundation of family dentistry. Regular exams, cleanings, fluoride treatments, and sealants reduce the risk of cavities and gum disease. Prevention not only saves money and time but also protects patients from pain and invasive procedures. According to the American Dental Association, preventive dentistry is the most effective approach to maintaining long-term oral health. Building Lifelong Oral Health Habits Family dentistry encourages healthy habits that last a lifetime. Children learn from their parents’ example, while teens gain independence in oral care routines. Adults continue preventive practices that protect their oral health and reduce risks as they age. Personalized Care Plans Each family member has unique dental needs. A family dentist creates individualized care plans based on
Family Dentistry in Fallbrook: Caring for Every Smile at Every Stage of Life

Main Takeaways: Family dentistry provides comprehensive dental care for all ages under one roof, from toddlers to seniors Long-term relationships with a family dentist lead to better monitoring of oral health changes and early problem detection Preventive care is the foundation of family dentistry, reducing the risk of major dental issues and saving time and money Convenient scheduling for multiple family members on the same day improves consistency with dental visits Early dental care for children builds positive habits and reduces dental anxiety throughout life Oral health is connected to overall health, with links to heart health, diabetes, and other systemic conditions Personalized care plans ensure each family member receives age-appropriate treatment and guidance What Is Family Dentistry Family dentistry provides dental care for patients of all ages. Instead of visiting different dentists for children, adults, and older family members, everyone can receive care under one roof. Family dentists are trained to treat a wide range of dental needs. These include cleanings, exams, fillings, crowns, gum care, and education tailored to each age group. This approach helps families stay consistent with dental visits and preventative care. Why Family Dentistry Matters for Long Term Oral Health Seeing the same dentist over time allows for better monitoring of oral health changes. A family dentist understands each patient’s dental history, habits, and risk factors. This long-term view helps catch problems early. Cavities, gum disease, and bite issues can often be treated more easily when found early. Family dentistry supports prevention rather than reaction. Family Dentistry in Fallbrook for Young Children Early dental care sets the foundation for lifelong oral health. Family dentistry in Fallbrook helps children feel comfortable in a dental setting from a young age. Dentists focus on gentle exams, education, and positive experiences. Kids learn how to brush and floss correctly and why dental care matters. These early visits help reduce dental anxiety later in life. Preventing Cavities in Children Children are more prone to cavities due to developing brushing habits and diets high in sugar. Family dentists provide cleanings, fluoride treatments, and sealants to protect young teeth. Education is also key. Parents receive guidance on nutrition, brushing routines, and habits like thumb sucking or pacifier use. Dental Care for Teens and Adolescents Teenagers face unique dental challenges. Orthodontic needs, sports-related injuries, and changing oral hygiene habits all play a role. Family dentistry in Fallbrook supports teens through these changes. Dentists monitor tooth alignment, wisdom tooth development, and gum health while encouraging independence in dental care. Supporting Busy Families With Convenient Scheduling One major benefit of family dentistry is convenience. Families can often schedule multiple appointments on the same day. This reduces missed school and work time while making it easier to stay on track with regular dental visits. Convenience leads to better consistency, which improves oral health over time. Preventive Dental Care for Adults Adults benefit from regular cleanings, exams, and preventive treatments. Family dentists help manage common adult dental issues like cavities, gum disease, and tooth wear. Routine care also helps identify problems linked to stress, grinding, or lifestyle factors. Early treatment can prevent more complex and costly procedures later. Gum Health and Periodontal Care Gum disease is common among adults and often develops without noticeable pain. Family dentistry focuses on early detection and treatment of gum issues. Regular cleanings and exams help prevent gingivitis from progressing into more serious periodontal disease. Healthy gums support overall oral health and tooth stability. Restorative Dentistry for the Whole Family When dental problems occur, family dentists provide restorative treatments to repair and protect teeth. These may include fillings, crowns, and bonding. Restorative care is tailored to each patient’s age and needs. The goal is to restore function while preserving as much natural tooth structure as possible. Dental Care for Seniors Oral health needs change with age. Seniors may face tooth wear, dry mouth, gum recession, or missing teeth. Family dentistry in Fallbrook addresses these concerns with gentle care and personalized treatment plans. Maintaining oral health supports nutrition, comfort, and overall quality of life. Monitoring Changes Over Time Seeing the same dental team year after year allows for better tracking of changes. Dentists can notice small shifts in bite, tooth wear, or gum health. This long-term insight leads to more accurate treatment planning and better outcomes. Family dentistry values continuity of care. Education and Communication for Every Age Education is a key part of family dentistry. Dentists explain procedures and preventive care in ways patients can understand. Children learn basics, teens learn responsibility, and adults receive guidance on maintaining oral health at home. Clear communication builds trust and confidence. Reducing Dental Anxiety for the Whole Family Dental anxiety affects both children and adults. Family dentistry focuses on creating a calm, welcoming environment. Familiar faces and routines help patients feel at ease. When families trust their dentist, they are more likely to attend regular visits and follow care recommendations. The Role of Technology in Family Dentistry Modern family dentistry uses updated technology to improve comfort and accuracy. Digital imaging, advanced tools, and efficient procedures enhance patient experience. Technology helps dentists diagnose problems earlier and plan treatments more precisely. This benefits patients of all ages. Family Dentistry in Fallbrook and Preventive Focus Preventive care is at the heart of family dentistry. Regular checkups, cleanings, and education reduce the risk of major dental problems. This approach saves time, money, and discomfort. Prevention keeps smiles healthy and strong over the long term. According to the American Dental Association, preventive dentistry is essential for maintaining optimal oral health throughout life. Building Lifelong Dental Habits Family dentistry helps build healthy habits that last a lifetime. When children see parents prioritizing dental care, they learn to do the same. These habits support better oral health into adulthood and beyond. Family dentistry encourages consistency and accountability. Personalized Care for Each Family Member Even within the same family, dental needs differ. Family dentists customize care plans for each patient. This personalized approach ensures that every family member receives appropriate treatment and
Where Can I Get Dental Implants Near Me in Torrance?
If you are missing one or more teeth, it is normal to feel unsure about what to do next. You may be asking yourself, where can i get dental implants near me in torrance, and how do I know I am choosing the right provider? Dental implants are one of the most trusted solutions for replacing missing teeth. They look natural, feel secure, and help protect your jawbone. Still, the process can feel overwhelming if you are unfamiliar with how implants work or what to look for in a dental office. This article explains what dental implants are, who they are for, what the process involves, and how to find a reliable implant provider in Torrance. By the end, you should feel more confident about taking the next step toward restoring your smile. What Are Dental Implants and How Do They Work? Dental implants are small titanium posts that are placed into the jawbone to replace missing tooth roots. Over time, the bone bonds with the implant, creating a strong foundation for a replacement tooth. Once the implant heals, a connector piece called an abutment is attached. A custom crown is then placed on top. The crown is designed to match the color and shape of your natural teeth. Unlike dentures, implants do not slip or move. Unlike bridges, they do not rely on nearby teeth for support. This makes them one of the most stable and long lasting tooth replacement options available. Why Dental Implants Are a Popular Choice in Torrance Many patients in Torrance choose dental implants because they offer both comfort and durability. Implants allow you to eat, speak, and smile without worrying about loose teeth. Dental implants also help prevent bone loss. When a tooth is missing, the jawbone in that area begins to shrink. Implants stimulate the bone and help maintain facial structure. Another reason implants are popular is their longevity. With proper care, they can last decades or even a lifetime. This makes them a smart long term investment in oral health. Who Is a Good Candidate for Dental Implants? Most healthy adults can be good candidates for dental implants. You may be a strong candidate if you: Have one or more missing teeth Have healthy gums Have enough jawbone to support an implant Are in good overall health Do not smoke heavily or are willing to quit Even if you have been told in the past that you are not a candidate, newer dental techniques may offer solutions. Bone grafting and advanced imaging allow more patients to qualify than ever before. A dental implant consultation is the best way to determine eligibility. Common Reasons People Lose Teeth Understanding why teeth are lost helps explain why implants are often recommended. Some common causes include: Tooth decay that cannot be repaired Gum disease Trauma or injury Failed root canals Cracked or broken teeth Congenital missing teeth Regardless of the cause, replacing missing teeth is important for oral health, not just appearance. What to Expect During the Dental Implant Process The dental implant process usually takes place over several months, but each step is carefully planned. Initial Consultation and Imaging The process begins with a detailed exam. This may include digital X rays or 3D imaging to evaluate bone density and placement options. Your dentist will review your health history, discuss treatment goals, and explain the recommended plan. Implant Placement During this step, the implant is surgically placed into the jawbone. Local anesthesia is used, and many patients report minimal discomfort. After placement, the implant needs time to heal and bond with the bone. This healing phase is called osseointegration. Abutment and Crown Placement Once healing is complete, the abutment is attached. A custom crown is then created and secured, restoring the look and function of your tooth. How Long Does It Take to Get Dental Implants? The timeline varies depending on individual needs. Some patients complete treatment in a few months. Others may need additional procedures that extend the timeline. Factors that affect timing include: Bone density Healing response Need for bone grafting Number of implants placed Your dentist will provide a clear timeline during your consultation. Dental Implants vs Other Tooth Replacement Options When asking where to get dental implants near me in Torrance, it helps to understand why implants are often preferred over other options. Dental Bridges Bridges rely on adjacent teeth for support. This requires reshaping healthy teeth and does not prevent bone loss. Dentures Dentures can be removable or fixed, but they may shift or feel uncomfortable. They also do not provide the same chewing strength as implants. Dental Implants Implants stand alone, preserve bone, and feel the most natural. They are often considered the gold standard for tooth replacement. What Makes a Good Dental Implant Provider in Torrance Choosing the right provider is just as important as choosing the treatment itself. Look for a dental office that offers: Experience with implant procedures Advanced diagnostic technology Personalized treatment plans Clear communication A focus on patient comfort A provider who explains your options clearly and answers your questions openly is a strong sign of quality care. Why Experience Matters with Dental Implants Dental implants require precision and planning. The placement angle, depth, and spacing all affect long term success. An experienced provider understands how to avoid complications and ensure proper healing. They also know how to handle complex cases involving bone loss or previous dental work. Experience leads to better outcomes and greater peace of mind. How Dental Implants Improve Daily Life Dental implants do more than replace missing teeth. They restore confidence and comfort in everyday activities. Patients often report improvements in: Chewing and digestion Speech clarity Self confidence Facial appearance Overall oral health Because implants feel like natural teeth, many patients forget they even have them. Cost Considerations for Dental Implants Dental implant costs vary depending on the number of implants and additional procedures needed. While implants may cost more upfront than other options, they often save money long
Do I Need a Bone Graft if I’m Not Getting an Implant?
Dental care is more than just routine cleanings and fillings. Sometimes, treatments like bone grafts are discussed even when a patient isn’t planning to get a dental implant. If you’ve ever wondered, do i need a bone graft if i’m not getting an implant, you’re not alone. Understanding why bone grafts are recommended and what alternatives exist can help you make informed decisions for your oral health. Bone grafting is commonly associated with dental implants, but it is not exclusive to them. There are multiple reasons a dentist might suggest a bone graft, even if you are not planning an implant. This article explores what bone grafts are, their purpose, alternatives, and factors to consider in your decision-making. What Is a Bone Graft? A bone graft is a dental procedure where material is added to your jawbone to support bone health and structure. This material can come from your own body, a donor, or synthetic sources. Bone grafting helps maintain or restore the shape and density of the jawbone. The main goal is to provide support for your teeth and facial structure. Even if you’re not getting an implant, maintaining adequate bone levels can prevent shifting teeth, gum recession, and changes in your facial appearance. Why Dentists Recommend Bone Grafts Dentists may recommend bone grafts for several reasons, not all related to implants: Prevent Bone Loss After Tooth Extraction When a tooth is removed, the surrounding bone may shrink over time. This can alter your smile and make future dental work more challenging. A bone graft can help preserve the jawbone’s shape. Support for Dentures or Bridges If you plan to wear dentures or bridges, a strong jawbone provides better fit and comfort. Bone grafts can prevent discomfort and reduce the risk of denture slippage. Maintain Facial Structure Loss of bone can lead to sunken cheeks and changes in your facial profile. Bone grafts can prevent these aesthetic issues, maintaining your natural appearance. Address Gum Disease Severe periodontal disease can cause bone loss around teeth. Grafting can help restore bone levels and support remaining teeth. When a Bone Graft Might Not Be Necessary Even though bone grafts have benefits, they aren’t always required. Your dentist will consider several factors: Current Bone Density: If your jawbone is healthy and dense, grafting may not be needed. Planned Dental Work: If you’re not getting implants, your existing teeth may provide sufficient support. Age and Health: Younger patients or those with good oral hygiene may not need grafts to prevent future problems. Extent of Bone Loss: Minor bone loss often does not require grafting, while significant loss may need intervention. Alternatives to Bone Grafting If you are unsure about getting a bone graft, there are alternatives to maintain jawbone health: Maintain Natural Teeth Regular dental checkups, brushing, and flossing prevent tooth loss and protect bone density. Healthy teeth stimulate the jawbone naturally. Use of Dentures or Bridges Without Grafts Modern dentures and bridges can be designed to fit well without requiring additional bone support in some cases. Orthodontic Treatments Orthodontic procedures can help align teeth and maintain jaw structure, reducing the need for grafting. Minimally Invasive Procedures In some cases, less invasive techniques such as socket preservation may help maintain bone levels after tooth extraction without full grafting. Risks and Considerations of Bone Grafts Like any procedure, bone grafting carries considerations: Infection: Rare, but possible if post-procedure care is inadequate. Discomfort and Swelling: Temporary discomfort is common after the procedure. Cost: Bone grafts can be expensive, especially if insurance does not cover them. Healing Time: Grafts require healing before full function is restored, which can take several months. Understanding these factors helps you weigh the benefits against potential downsides. Signs You May Benefit from a Bone Graft Even if you’re not planning an implant, certain signs indicate that a bone graft might improve oral health: Noticeable bone loss or shrinking gums Loosened teeth due to bone loss Difficulty wearing dentures Significant tooth extraction sites that have not healed fully A dental professional can evaluate your jawbone through X-rays or CT scans to determine if grafting is beneficial. How Bone Grafts Can Prevent Future Dental Problems Bone grafts are proactive treatments. They can prevent: Tooth shifting that leads to bite problems Gum recession and exposure of tooth roots Facial changes caused by bone loss Complications if future implants or other dental procedures are desired Even if you currently have no plans for implants, preserving bone now can make future dental care simpler and less costly. What to Expect During a Bone Graft Procedure A bone graft procedure typically involves: Assessment: Dental imaging evaluates the jawbone. Preparation: Local anesthesia or sedation is administered. Placement: Bone material is added to areas of bone loss. Stabilization: Membranes or screws may be used to hold graft material in place. Healing: The graft integrates with the existing bone over several months. Dentists provide aftercare instructions to ensure proper healing and reduce risks of infection or complications. Recovery and Aftercare for Bone Grafts Proper aftercare is essential for successful grafting: Maintain oral hygiene with gentle brushing and rinsing Avoid hard or sticky foods during initial healing Take prescribed medications to prevent infection and manage pain Attend follow-up appointments to monitor bone integration Following these guidelines improves the likelihood of a successful procedure and reduces discomfort. Consulting With Your Dentist The decision to get a bone graft should be made with guidance from a qualified dental professional. Questions to ask include: What are the long-term benefits if I’m not getting an implant? Are there non-surgical alternatives that meet my needs? How will this procedure affect my current and future dental plans? What are the costs and expected recovery time? A thorough consultation ensures that you understand both the necessity and implications of grafting. Cost Considerations for Bone Grafting Bone graft costs vary depending on the procedure’s complexity, materials used, and location. Some dental insurance plans cover bone grafts if they are deemed medically necessary. Discussing financial aspects with your dentist helps

